Groin Pain
- No painful injections
- No unnecessary surgery
- No expensive medications
Groin Pain
- No painful injections
- No unnecessary surgery
- No expensive medications
- Community-Based Physical Activity Programs for Arthritis
- Osteoarthritis
- Rheumatoid Arthritis
What is Osteoarthritis of the Hip?
How Does Hip Arthritis Feel?
- Sharp, shooting pain or dull, achy pain in the hip, groin, thigh, knee, or buttocks
- Stiffness in the hip joint, which is worse after sleeping or sitting
- A “crunching”; sound when the hip joint is moved, caused by bone rubbing on bone
- Difficulty and pain when getting out of bed, standing up from a sitting position, walking, or climbing stairs
- Difficulty performing normal daily activities, such as putting on socks and shoes
How Is Hip Arthritis Diagnosed?
- When and how frequently do you feel pain and/or stiffness?
- What activities in your life are made difficult by this pain and stiffness?
- Gently moving your leg in all directions (range of motion test)
- Asking you to resist against her hand as she tries to gently push your leg and hip in different directions (muscle strength test)
- Watching you walk to check for limping
- Asking you to balance while standing (balance test)
How Can a Physical Therapist Help Treat Arthritis in the Hip?
- Reduce your pain
- Improve your leg, hip, and back motion
- Improve your strength, standing balance, and walking ability
- Speed healing and your return to activity and sport
Can Hip Arthritis be Prevented?
What is Hip Impingement?
- In pincer-type impingement, the hip socket (acetabulum), which is usually angled forward, may be angled toward the back, or protruding bone may be present on the pelvis side of the hip joint making the socket a deeper recess that covers more of the ball or head of the femur bone.
- The overgrown bone or incorrect angle of the socket causes the labrum, a rim of connective tissue around the edge of the hip socket, to be pinched. Over time, this extra pressure to the labrum when flexing (moving the leg forward) leads to wear and tear that can cause inflammation and could result in a tear. If this condition persists, eventually the cartilage that lines the hip joint can become worn and form holes.
- This condition affects men and women equally; symptoms often begin early, appearing at any time between 15 to 50 years of age.
- In cam-type impingement, the shape of the bone around the head of the femur—the ball at the top of the bone in the thigh—is misshapen. It can vary from the normal round ball shape, or have overgrown bone formed at the top and front. The nickname “pistol grip” deformity is given to the appearance of the bony overgrowth on x-rays.
- The overgrown or misshapen bone contacts the cartilage that lines the hip socket, and can cause it to peel away from the bone in the socket. The labrum can become worn, frayed, or torn as well.
- This condition affects men to women at a ratio of 3 to 1; symptoms often manifest during the teen years and 20s.
Signs and Symptoms of Hip Impingement
Hip impingement may cause you to experience:- Stiffness or deep aching pain in the front or side of the hip or front of the upper thigh while resting.
- Sharp, stabbing pain when standing up from a chair, squatting, rising from a squat, running, “cutting,” jumping, twisting, pivoting, or making lateral motions.
- Hip pain described in a specific location by making a “C” with the thumb and hand and placing it on the fold at the front and side of the hip, known as the “C-sign.”
- Pain that most often starts gradually, but can also remain after another injury resolves.
- Pain that increases with prolonged sitting or forward leaning.
- Feeling less flexible at the hips, including a decreased ability to turn your thigh inward on the painful side.
How Is Hip Impingement Diagnosed?
How Can a Physical Therapist Help Treat Hip Impingment?
Without Surgery- Improving the strength of your hips and trunk. Strengthening of the hips and trunk can reduce abnormal forces on the already injured joint and help with strategies to compensate.
- Improving hip muscle flexibility and joint mobility. Stretching tight muscles can reduce abnormal forces that cause pain with motion. Joint mobilization may help ease pain from the hip joint; however, these treatments do not always help range of motion, especially if the shape of the bone at the hip joint has changed.
- Improving tolerance of daily activities. Your physical therapist can consider your job and recreational activities and offer advice regarding maintaining postures that are healthier for your hip and activity modification. Often this involves limiting the amount of bending at the hip to avoid further hip damage.
- Ensuring your safety as you heal. Your physical therapist may recommend that you limit the amount of weight you put on the operated leg if there was a repair of the labrum. You may wear a brace to help limit the amount of bending at the hip. You might also use crutches to avoid overloading the leg if the bone on the femur was reshaped.
- Improving your range of motion, strength, and balance. Your physical therapist will guide you through safe range-of-motion, strengthening, and balance activities to improve your movement as quickly as possible while allowing the surgical site to heal properly.
- Instructions on returning to an active lifestyle. Most people return to normal daily activities about 3 months after surgery, and to high-level activities and sports 4 to 6 months after surgery. Your physical therapist will recommend a gradual return to activity based on your condition—research shows that 60% to 90% of athletes return to their previous playing ability depending on the surgical procedure performed and the sport.
Can Hip Impingement be Prevented?
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, and It's Free!

- Learn The Essential First Step... So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results!
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
Solve the root cause of your pain
How Our Treatment is Different
We believe that working with a specific specialist for your care is the best way to solve the root cause of your pain. Work one-on-one with a Doctor of Physical Therapy every time your visit our office.
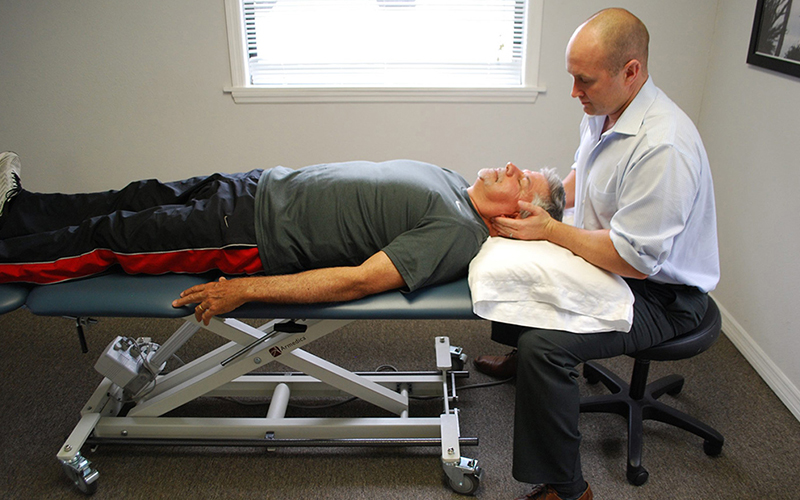
Exclusive one-on-one patient care
While most clinics will give you a limited amount of time with your Doctor, we believe that true results come from consistent one-on-one therapy.
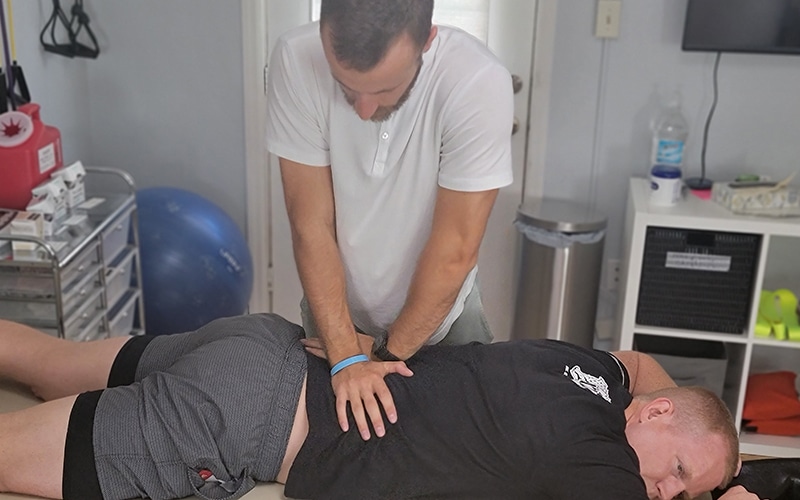
Work with your specialist every visit
Stop being handed off to trainees or non-Doctors for your Physical Therapy. At Pursuit, you'll work exclusively with your Doctor of Physical Therapy that specializes in your specific needs.
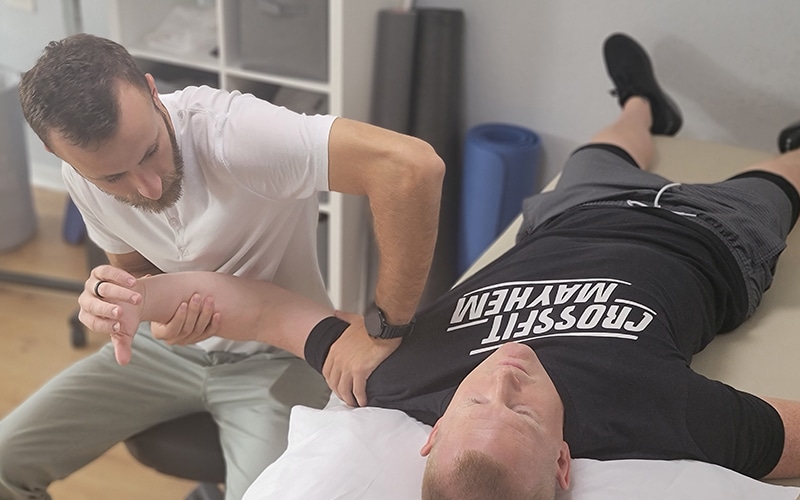
24/7 messaging access to your specialist
Ever have an issue or questions? We're here to help. Get 24/7 access to your specialist while you're under our care. Physical Therapy doesn't just happen when you're in our clinic, so we're here for you when you need us.
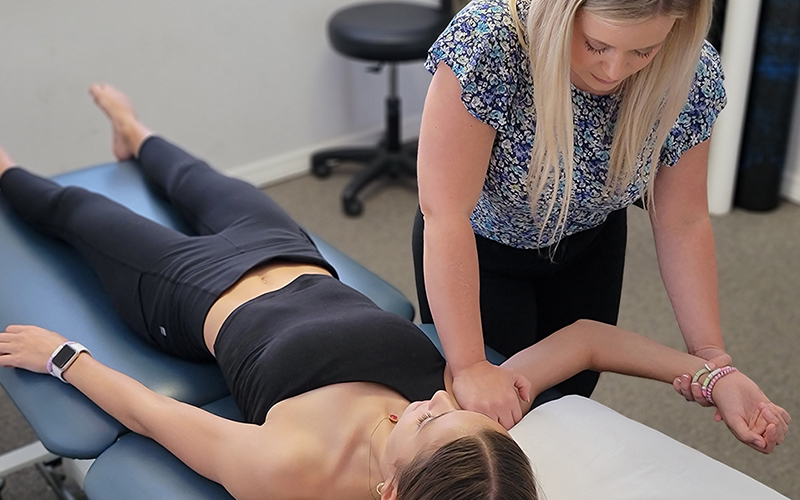
No waiting periods
Get off that waiting list and get the treatment you need. We're always ready to accept new patients, so you can get better faster and get back to a pain-free life that you deserve.
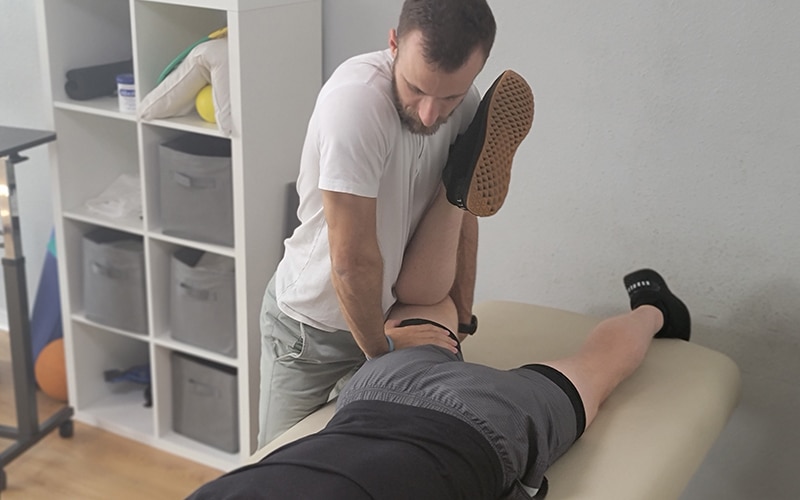
Not limited by insurance
Don't let the insurance companies tell you how much treatment you need. Avoid the limitations of short sessions that insurance provides and work with our Doctors when you need it and for as long as you need it.
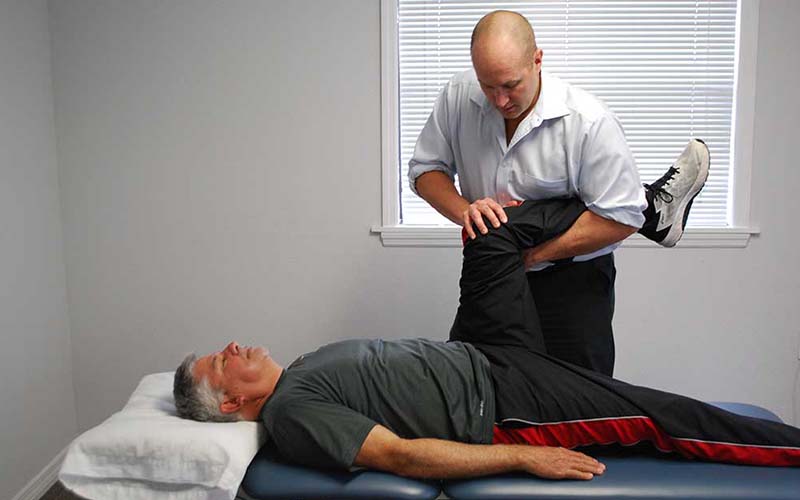
No painful injections, no expensive medications, no surgery
In order to truly solve your pain, we use a holistic approach to Physical Therapy, not relying on injections, medications, or surgery. Instead, we'll strengthen your body's weak points that are causing your pain.
MEET THE TEAM

RON MILLER, DPT, OCS, Cert DN
Doctor of Physical Therapy | Board Certified Orthopaedic Physical Therapy Clinical Specialist | Post-Doctoral Orthopaedic Residency Trained | Certified in Dry Needling | Titleist Performance Institute Certified
Dr. Ron Miller is the owner and founder of Pursuit Physical Therapy. His core belief is that it is not about the physician, the physical therapist, or the insurance company: it is about what is truly best for the patient. Dr. Miller started...

CAREY ROTHSCHILD, DPT, OCS, SCS, CSCS, CKTP
Doctor of Physical Therapy and Assistant Professor at the University of Central Florida | Board Certified Orthopaedic Clinical Specialist
| Board Certified Sport Clinical Specialist
Dr. Carey Rothschild is an Assistant Clinical Professor in the Doctor of Physical Therapy Program at the University of Central Florida. Dr. Rothschild earned a Bachelor of Health Science in Physical Therapy in 1999 from the University of Florida and a Doctor of Physical Therapy from Boston University in 2005...


MICHAEL FABRICK, DPT, Cert. DN
Doctor of Physical Therapy | Certified in Dry Needling | Pursuit Sports Performance Specialist | Professional Tennis Tour Physical Therapist
Dr. Michael Fabrick was born and raised in Hanover, Pennsylvania and attended Slippery Rock University where he received his Bachelor’s degree in Exercise Science. He then went on to receive his Doctorate Degree in Physical Therapy in May of 2020. During his final tenure as a Doctoral intern, he trained underneath Todd Ellenbecker, who is one of the world’s leading experts on shoulder rehabilitation and is the Vice President of Medical Services for the ATP World Tour...

MARYANN DANIELS, PT, MCMT, IDN
Physical Therapist | Dry Needling Certified | Mastery Certified In Manual Therapy | Pelvic Floor And Post Partum Specialist
Maryann was originally born in Connecticut but moved to Florida with her family at the age of 9 and she grew up in Jupiter, Florida. She then went to college at the University of Central Florida...


Kayla Cook, DPT, HSP, CSCS
Doctor of Physical Therapy | Hesch Sacroiliac Practitioner | Certified Strength And Conditioning Specialist | Ehlers-Danlos Syndrome Specialist | Volleyball Specialist
Dr. Kayla Cook was born and raised in Northern California and received her undergraduate degree in Kinesiology from California State University in Sacramento. She then received her Doctorate in Physical Therapy from The University of St Augustine for Health Sciences...
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, And It's Free!

- Learn The Essential First Step...So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
BECOMING PAINFREE IS EASIER THAN YOU THINK

Step 1:
Call our expert team.

Step 2:
We’ll work with you to find and treat the root of your pain.

Step 3:
Get back to doing what you love.
