Clicking in the Knee
- No painful injections
- No unnecessary surgery
- No expensive medications
Clicking in the Knee
- No painful injections
- No unnecessary surgery
- No expensive medications
What is a Meniscal Tear?
Signs and Symptoms of a Meniscus Tear
- Feel a sharp, intense pain in the knee area
- Feel a “pop” or a tearing sensation
- Have difficulty walking because of pain or a “catching” sensation
- Have difficult straightening the knee
- Experience swelling within the first 24 hours of injury
How Is a Meniscus Tear Diagnosed?
- Conduct a thorough evaluation that includes a detailed review of your injury, your symptoms, and your health history
- Perform special tests to measure the range of motion (amount of movement) in your knee and determine which specific movements and positions increase your symptoms
- Use a series of tests that apply pressure to the meniscus to determine whether it appears to be damaged
How Can a Physical Therapist Help treat a Meniscus Tear?
Can a Meniscus Tear be Prevented?
- Regular exercise helps strengthen the muscles that support your knees.
- Staying physically active helps prepare your body for the demands of a sport or strenuous activity.
- Although accidents are difficult to prevent, avoiding twisting or turning quickly while your foot is planted may help prevent meniscal tears.
What is Patellofemoral Pain or Anterior Knee Pain?
- Weakness, tightness, or stiffness in the muscles around the knee
- An abnormality in the way the lower leg lines up with the hip, knee, and foot
- Feel pain after sitting for long periods of time with the knee bent
- Occasionally hear or feel a “cracking” or “popping” when you bend or straighten your kne
How Is Patellofemoral Knee Pain Diagnosed?
Your physical therapist will review your health history, perform a thorough examination, and conduct a series of tests to evaluate the knee. Physical therapists use tests such as the patellar apprehension test, the Q-angle test, the patella alta test, and Clarke’s sign (patellar grind test) to determine whether the patellofemoral joint is the source of pain. In addition, your therapist may observe the alignment of your feet, analyze your walking and running patterns, and test the strength of your hip and thigh muscles to find out whether there is a weakness or imbalance that might be contributing to your pain. Finally, your therapist will check the flexibility of the muscles in your leg, paying close attention to those that attach at the knee. Generally, x-rays are not needed to diagnose PFPS.How Can a Physical Therapist Help Treat Patellofemoral Knee Pain or Anterior Knee Pain?
- Strengthening exercises targeted at the hip (specifically the abductor and rotator muscles of the buttock and thigh), the knee (specifically the quadriceps femoris muscle, which is located on the front of your thigh and straightens your knee), and the ankle
- Stretching exercises for the muscles of the hip, knee, and ankle
- Taping of the patella to reduce pain and retrain muscles to work efficiently
- Exercises for improving your performance of activities that have become difficult for you
- Have you try a lightweight brace
- Use pain-reducing treatments such as electrical stimulation
- Recommend that you apply ice or heat at home for relief
Can Patellafemoral Knee Pain be Prevented?
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, and It's Free!

- Learn The Essential First Step... So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results!
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
Solve the root cause of your pain
How Our Treatment is Different
We believe that working with a specific specialist for your care is the best way to solve the root cause of your pain. Work one-on-one with a Doctor of Physical Therapy every time your visit our office.
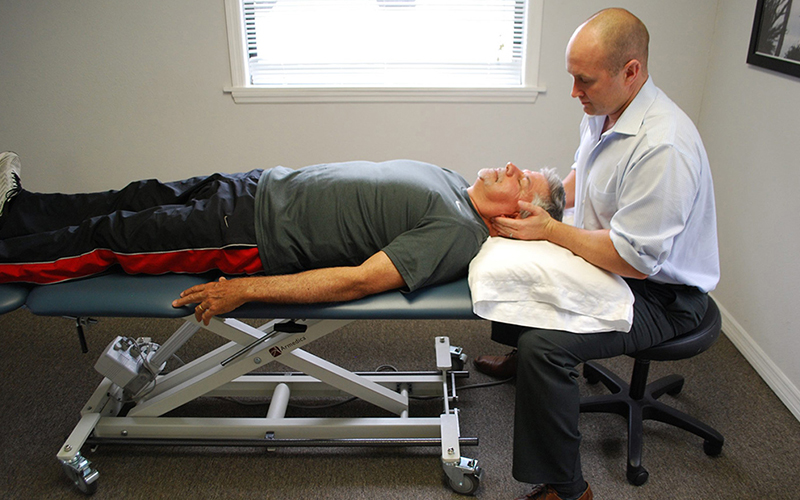
Exclusive one-on-one patient care
While most clinics will give you a limited amount of time with your Doctor, we believe that true results come from consistent one-on-one therapy.
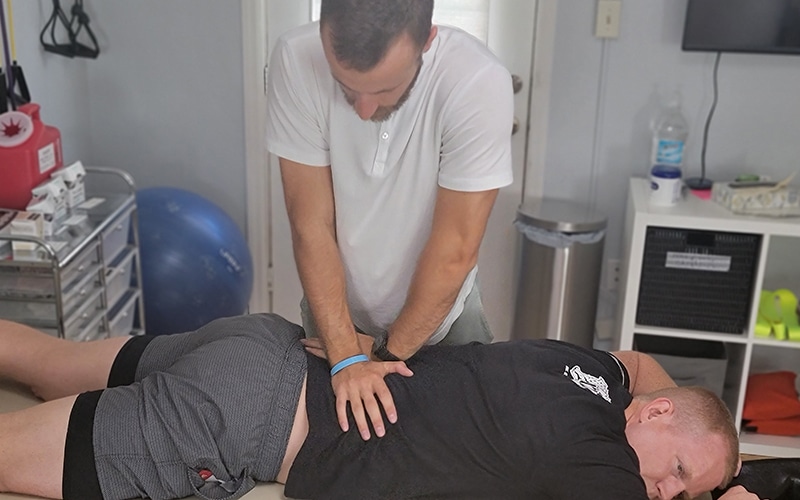
Work with your specialist every visit
Stop being handed off to trainees or non-Doctors for your Physical Therapy. At Pursuit, you'll work exclusively with your Doctor of Physical Therapy that specializes in your specific needs.
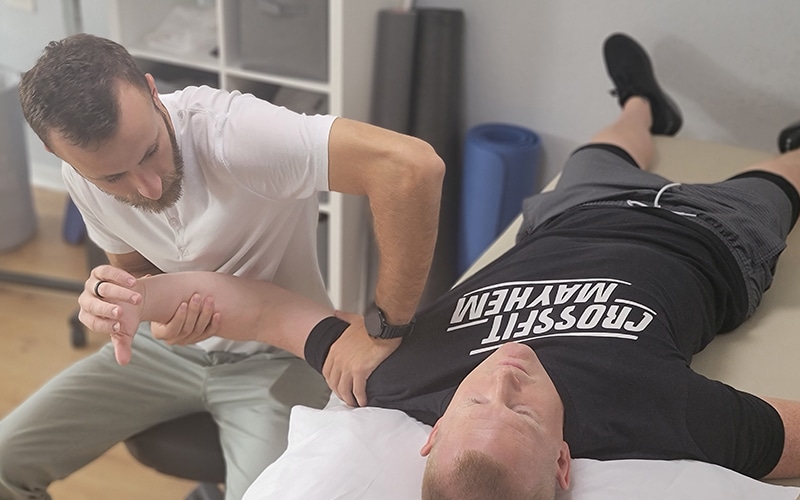
24/7 messaging access to your specialist
Ever have an issue or questions? We're here to help. Get 24/7 access to your specialist while you're under our care. Physical Therapy doesn't just happen when you're in our clinic, so we're here for you when you need us.
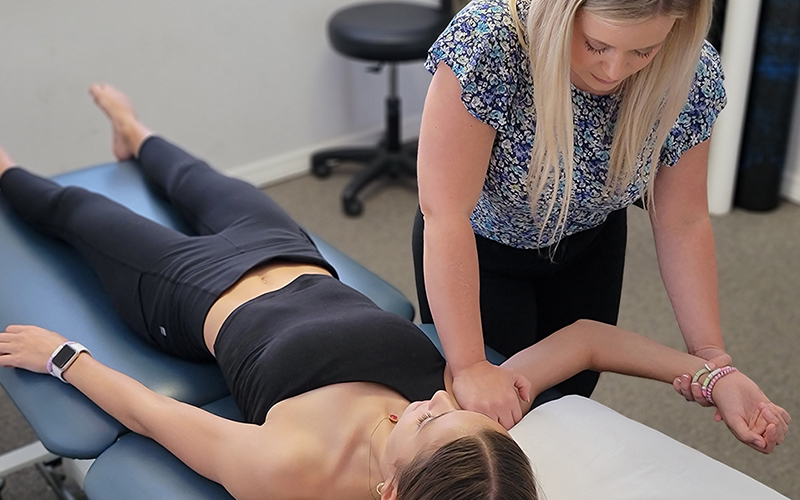
No waiting periods
Get off that waiting list and get the treatment you need. We're always ready to accept new patients, so you can get better faster and get back to a pain-free life that you deserve.
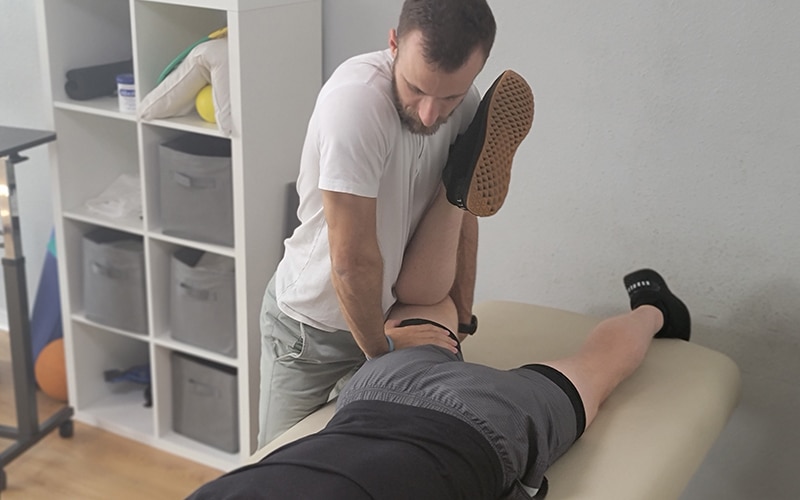
Not limited by insurance
Don't let the insurance companies tell you how much treatment you need. Avoid the limitations of short sessions that insurance provides and work with our Doctors when you need it and for as long as you need it.
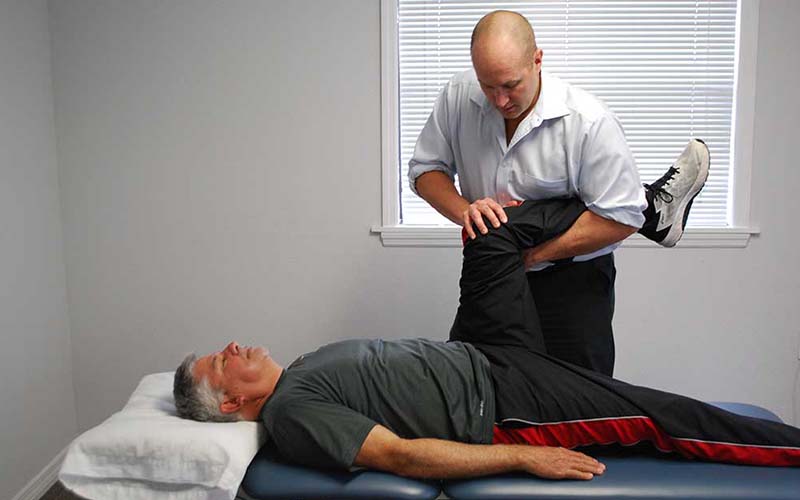
No painful injections, no expensive medications, no surgery
In order to truly solve your pain, we use a holistic approach to Physical Therapy, not relying on injections, medications, or surgery. Instead, we'll strengthen your body's weak points that are causing your pain.
MEET THE TEAM

RON MILLER, DPT, OCS, Cert DN
Doctor of Physical Therapy | Board Certified Orthopaedic Physical Therapy Clinical Specialist | Post-Doctoral Orthopaedic Residency Trained | Certified in Dry Needling | Titleist Performance Institute Certified
Dr. Ron Miller is the owner and founder of Pursuit Physical Therapy. His core belief is that it is not about the physician, the physical therapist, or the insurance company: it is about what is truly best for the patient. Dr. Miller started...

MARYANN DANIELS, PT, MCMT, IDN
Physical Therapist | Dry Needling Certified | Mastery Certified In Manual Therapy | Pelvic Floor And Post Partum Specialist
Maryann was originally born in Connecticut but moved to Florida with her family at the age of 9 and she grew up in Jupiter, Florida. She then went to college at the University of Central Florida...


MICHAEL FABRICK, DPT, Cert. DN
Doctor of Physical Therapy | Certified in Dry Needling | Pursuit Sports Performance Specialist | Professional Tennis Tour Physical Therapist
Dr. Michael Fabrick was born and raised in Hanover, Pennsylvania and attended Slippery Rock University where he received his Bachelor’s degree in Exercise Science. He then went on to receive his Doctorate Degree in Physical Therapy in May of 2020. During his final tenure as a Doctoral intern, he trained underneath Todd Ellenbecker, who is one of the world’s leading experts on shoulder rehabilitation and is the Vice President of Medical Services for the ATP World Tour...

THOMAS EBERLE, DPT, FAAOMPT
Doctor Of Physical Therapy | Fellow, American Academy Of Orthopedic Manual Physical Therapist | Dry Needling Certified |
Dr. Thomas Eberle is a native of Buffalo, New York where he completed his Master of Science, Physical Therapy from D’Youville College. Dr. Eberle went on and further completed his Doctor of Physical Therapy, an Orthopedic Residency, and a Fellowship program...

To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, And It's Free!

- Learn The Essential First Step...So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
BECOMING PAINFREE IS EASIER THAN YOU THINK

Step 1:
Call our expert team.

Step 2:
We’ll work with you to find and treat the root of your pain.

Step 3:
Get back to doing what you love.
