Best Orlando Treatment for a
PINCHED NERVE IN NECK
Are you not able to continue your cherished hobbies or everyday activities because of sharp pain in your neck when you move? With our expert doctors’ help, you can get to the root of your symptoms and get back to doing what you love quicker and easier.
Read More Ask A QuestionBest Orlando Treatment for a
PINCHED NERVE IN NECK
Are you not able to continue your cherished hobbies or everyday activities because of sharp pain in your neck when you move? With our expert doctors’ help, you can get to the root of your symptoms and get back to doing what you love quicker and easier.
Read More Ask A QuestionHere Is Everything You Need To Know About A Pinched Nerve In Your Neck, What Causes It, and The Best Way to Treat It
Click the tabs below to get direct answers to your questions
What is a pinched nerve?
A pinched nerve, also medically called cervicalgia or a cervical radiculopathy, occurs when a nerve root coming off the spinal cord becomes compressed. The cervical spine consists of 7 cervical vertebrae (the bones that form the neck region). Each vertebra is separated by a gel-like disc. The discs provide shock absorption for the spine. The spinal cord is like a tree trunk, and the spinal nerves are like the tree branches. If an impingement or abnormal pressure is placed on a branch near the trunk, everything along that branch will be affected. The compression can occur for various reasons. In younger people, it may occur when a cervical disc herniates due to trauma. In older individuals, it commonly occurs spontaneously as a result of arthritis or decreased disc height in the neck region. Spinal nerves can be impinged by:- Arthritis
- Disc wear-and-tear with age
- Herniated or bulging discs from trauma or degeneration
- Spinal stenosis (a narrowing of the spaces in which the nerves travel)
- Tumor (either benign or malignant)
What are common causes of a pinched nerve in the neck?
There are many common causes of a pinched nerve, especially after major medical red flags are ruled out:- Sleeping in an awkward neck position
- Being in an auto accident with whiplash
- Poor sitting posture at your computer or desk
- Improper heavy-lifting techniques
- Turning your neck to the side with poor posture
- Prolonged watching TV in a bad position
- Flying in an uncomfortable seat on an airplane
- Sport injury
- Sleeping with a bad pillow
Where does it hurt?
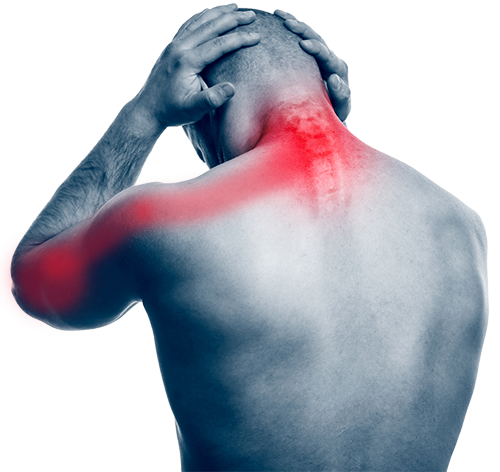 Your nervous system is a lot like a tree, with the ‘base’ of the tree near your neck and the ‘branches’ running through the rest of your body.
Because of this, it’s possible to feel the effects of a pinched nerve in other parts of your body besides your neck.
Understanding the root cause of your pain is fundamental approach to treating your pain in the long run & will decrease your dependence on painkillers or treatment that only address the symptoms.
Your nervous system is a lot like a tree, with the ‘base’ of the tree near your neck and the ‘branches’ running through the rest of your body.
Because of this, it’s possible to feel the effects of a pinched nerve in other parts of your body besides your neck.
Understanding the root cause of your pain is fundamental approach to treating your pain in the long run & will decrease your dependence on painkillers or treatment that only address the symptoms.
How do I know if I have a pinched nerve in my neck?
Symptoms of a pinched nerve vary depending on the nerve root involved, and commonly occur on the same side of the body as the affected nerve. The symptoms may include:- Pain in the neck, shoulder blade, shoulder, upper chest, or arm, with pain possibly radiating into the fingers following the path of the involved nerve root.
- Pain described as “sharp” or “pins-and-needles” or “popping sensation” in cervical region.
- General dull ache or numbness anywhere along the pathway of the nerve.
- Weakness in the shoulder, arm, or hand.
- Pain that worsens with certain neck movements.
- Pain that improves when the arm is lifted over and behind the head (relieving tension on the spinal nerve).
- C5 nerve root (between cervical vertebrae C4-C5): weakness in the deltoid muscle (front and side of the shoulder) and upper arm; shoulder pain and numbness
- C6 nerve root (between cervical vertebrae C5-C6): weakness in the bicep muscle (front of the upper arm) and wrist muscles; numbness on the thumb side of the hand
- C7 nerve root (between cervical vertebrae C6-C7): weakness in the triceps muscle (the back of the upper arm and wrist); numbness and tingling in the back of the arm and the middle finger of the affected hand
- C8 nerve root (between vertebrae C7-T1): weakness with hand grip; numbness in the little finger
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, and It's Free!

- Learn The Essential First Step... So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results!
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, And It's Free!

- Learn The Essential First Step...So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
Can a pinched nerve in the neck be treated?
Yes, a pinched nerve can be treated and with great results. Even better, many times it can be treated conservatively without needing injections, pain medications, or surgeries. The key to treatment is to solve the root cause of what is actually occurring at the neck that is causing your pinched nerve symptoms. Some root causes of a pinched nerve can be:- A herniated disc
- A hypomobile facet joint
- Decrease neck range of motion causing pinching
- Thoracic outlet syndrome
- Neck protrusion and poor posture
What happens if it goes untreated?
If you don’t get treatment for your neck pain, there are two possible outcomes. Minor case – If it is a minor injury, research shows that many acute cases of neck pain may spontaneously go away in 4-8 weeks. However, we still recommend that you get it checked out by a physical therapist to ensure that it is just a minor case. Severe case – If it is a more severe injury, your pain will start to worsen due to the compression on the nerve. The neck pain will increase because the root cause is not being treated. Many people turn to pain medication now but this only blocks the pain, but the pinched nerve is still there being pinched. Many people say after the pain medication is stopped, then usually the pain returns and sometimes it returns even worse. If the nerve is severely pinched, you may start to get referred pain into your shoulder blade area, shoulder, arm and into your hand, a headache, with a severe loss of neck range of motion to the side of the neck pain. If this continues to go untreated you may start experiencing neurological symptoms such as numbness and tingling, electric pain, muscle weakness, and a loss of reflexes. If it persists to this stage and left untreated, many people don’t respond to conservative treatments and may need surgery at this stage due to the neurological symptoms. If treated early and properly, surgery can be avoided and conservative treatments (ex. Manual therapy, stretching, joint mobilizations, and exercise) can show successful results. This is why it is crucial to take action early and resolve it before it gets to a chronic injury and doesn’t just hope your pain is going to go away. Research supports that early interventions lead to faster results and less time in pain.What outcome can you expect from treatment?
The treatment outcome after a pinched nerve can vary depending on the medical professional you choose, their treatment approach, your participation and effort, and the severity of the pinched nerve. If you have an acute pinched nerve case: You should recover fast (within weeks) as treatment starts. With each session, pain should start to decrease and you should start to regain and increase your neck range of motion. Your radicular or radiating symptoms should resolve fast too. Gradually you will regain full neck range of motion and the pain should be almost resolved by then. Within a matter of 2-4 weeks, you should have a full range of motion, minimal to no pain, great strength, and the underlying risk factors are resolved. By 2-6 weeks depending on your case, you can return to your normal activities, sport, and your favorite hobbies. Overall, if treated correctly, this is an easy case, with great results, and you should recover fully. If you have a chronic pinched nerve case that has been going on for months or years: You can still get a great outcome, it just takes longer and more effort. First, we have to solve the root cause of your pain, de-sensitize the nervous system, decrease fear-avoidance beliefs, and then you should start seeing a decrease in pain within weeks. The next step is to restore joint mobility and range of motion. This will further decrease your pain and you should start noticing that you can turn your head farther and you have fewer days with severe pain. The next step is to start strengthening and to maximize your range of motion so a full active range of motion can be reached. This will strengthen your new full range of motion, help prevent re-injury, and get you back to your favorite activities without worrying whether your neck will be in pain. Many chronic cases can show a 75-100% recovery. It just takes time and every case is different. Some chronic cases may take as fast as 2 months and as long as 4-6 months. Regardless, you can still get a great outcome and the results your desire, if treated properly.To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, and It's Free!

- Learn The Essential First Step... So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results!
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, And It's Free!

- Learn The Essential First Step...So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
How is it diagnosed?
When you seek the help for a pinched nerve, the clinician will perform a comprehensive evaluation and ask questions about your pain and your daily activities. These may include:- How and when the pain started: Did the pain begin spontaneously or was there any trauma or popping experienced in the cervical region?
- Where are the symptoms located, and have they changed location or intensity since the onset?
- What makes the symptoms better or worse?
- What type of work do you perform?
- What hobbies or household activities do you regularly perform?
How can a Physical Therapist treat it?
How long does it take for a recovery?
Recovery time for a pinched nerve in the neck depends on multiple factors: the severity of your pinched nerve, how long you have been in pain for, the medical professional you choose, and how active you are in trying to resolve your pain. If you do nothing, acute cases may or may not resolve in 4-8 weeks spontaneously. If you get expert treatment, some cases resolve in 1-3 weeks and get you back to the sport, exercise, and your favorite activities without flare-ups and recurrences. If it is a complex case of chronic pain, this may take longer, but you can still get a good outcome. Some chronic cases can resolve as fast as 2 months and as long as 4-6 months. It varies with every patient because every case of neck pain or a pinched nerve is different.How much does it cost?
The average cost of care for a case of spine pain in the US is $1800-$6600. This high price is thanks to the often inefficient and cumbersome approach to getting treated, often requiring multiple visits to different doctors and physical therapists until you get settled in and start treatment. We strive to end that unnecessary, expensive cycle. In fact, we are currently publishing our first-year data with the University of Central Florida that shows the cost-effectiveness of our treatment approach. The average cost of our care was shown to be $814. So if you have a deductible of $3000-$8,000, we can save you lots of money. Remember, every case of neck pain is different and not all neck pain is the same. So it is hard to predict and tell you how much your neck pain is going to cost you. But after a thorough evaluation, we can tell you exactly what is causing your neck pain, how long it is going to take, what is the best way to treat it, and exactly how much it is going to cost. We have no hidden fees, no co-pays, and no miscellaneous bills that you surprisingly receive 3 months later after you receive treatment. Your pain, your diagnosis, your goals, and what is best for you dictates your treatment and how much it will cost. It varies for every patient but it is still way cheaper than standard healthcare.How long are sessions?
Our evaluations are 60-90 minutes long. We like to perform thorough evaluations so we can solve the root cause of your pain, identify all risk factors, and make sure that we do it right. After the evaluation, you will know your diagnosis, the root cause of why you have your pain and symptoms, your prognosis, an expected timeline of when you should see results, what the best way to treat your pain is, how much it will cost, and your expected recovery. We will have plenty of time for you to ask questions and make sure you fully understand why you have your pain and what is the best way to treat it. After the evaluation is completed, all treatment sessions are 60 minutes going forward and you and your physical therapist will design a customized treatment plan that works for you and that will achieve your goals.How can it be prevented?
Your physical therapist will educate you on the best ways to prevent cervical radiculopathy from recurring, including:- Maintaining proper posture. Use a supportive pillow and proper posture when sitting at a desk or in the car.
- Setting up your workstation to minimize undue forces on the spine. You may be advised to use a hands-free phone or adjust your computer monitor to avoid excessive twisting or extending of your neck in repetitive directions during the workday.
- Continuing with regular exercise to maintain spinal muscles flexibility and strength, including the upper body, middle back, and core muscles.
- Keeping a healthy weight to minimize unnecessary forces on the spine.
What are next steps?
If you’re ready to get pain free, give us a call at (407) 494-8835 or fill out the form below. We’re happy to answer any questions and get you back to doing what you love.Solve the root cause of your pain
How Our Treatment is Different
We believe that working with a specific specialist for your care is the best way to solve the root cause of your pain. Work one-on-one with a Doctor of Physical Therapy every time your visit our office.
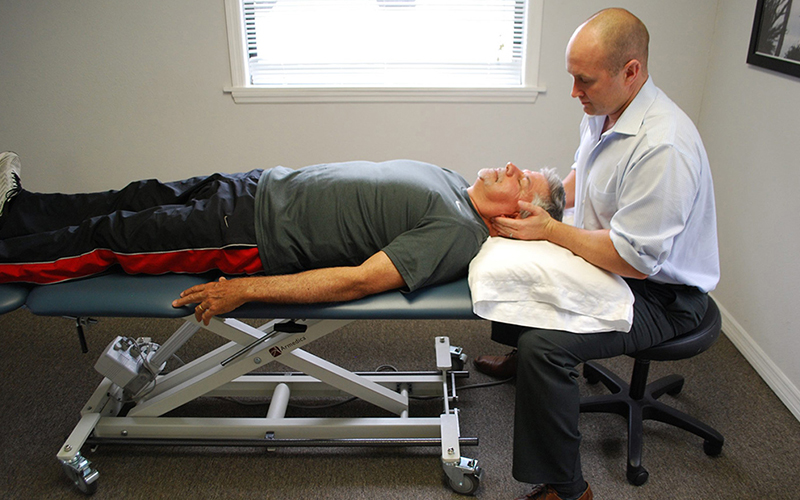
Exclusive one-on-one patient care
While most clinics will give you a limited amount of time with your Doctor, we believe that true results come from consistent one-on-one therapy.
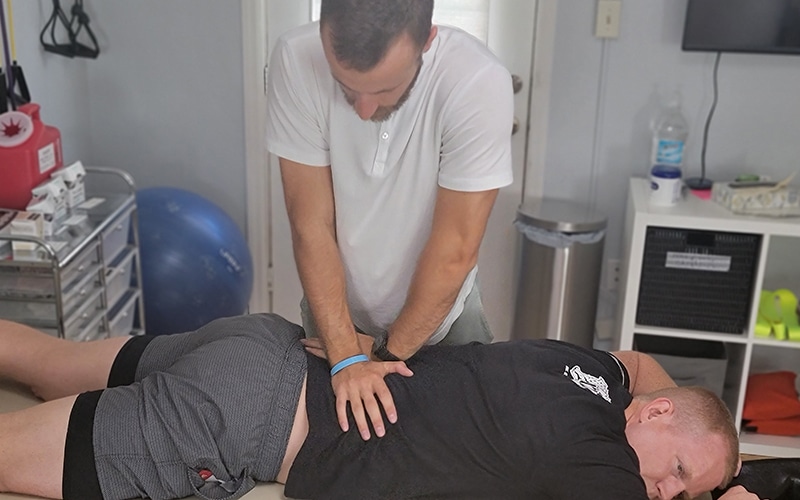
Work with your specialist every visit
Stop being handed off to trainees or non-Doctors for your Physical Therapy. At Pursuit, you'll work exclusively with your Doctor of Physical Therapy that specializes in your specific needs.
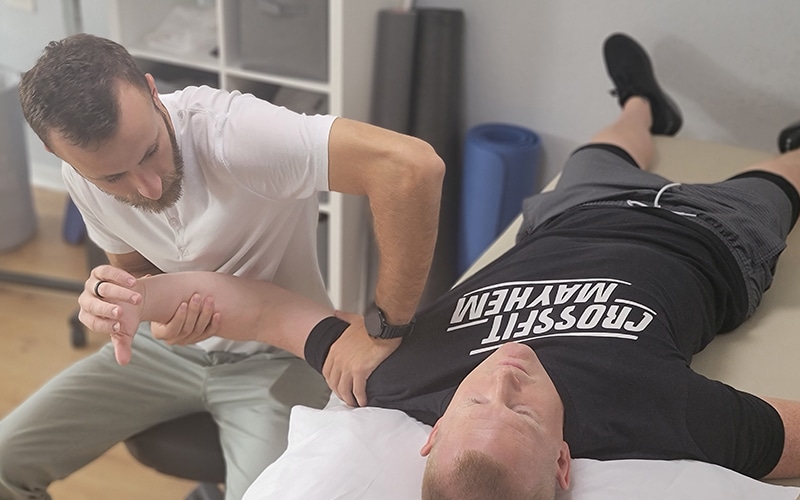
24/7 messaging access to your specialist
Ever have an issue or questions? We're here to help. Get 24/7 access to your specialist while you're under our care. Physical Therapy doesn't just happen when you're in our clinic, so we're here for you when you need us.
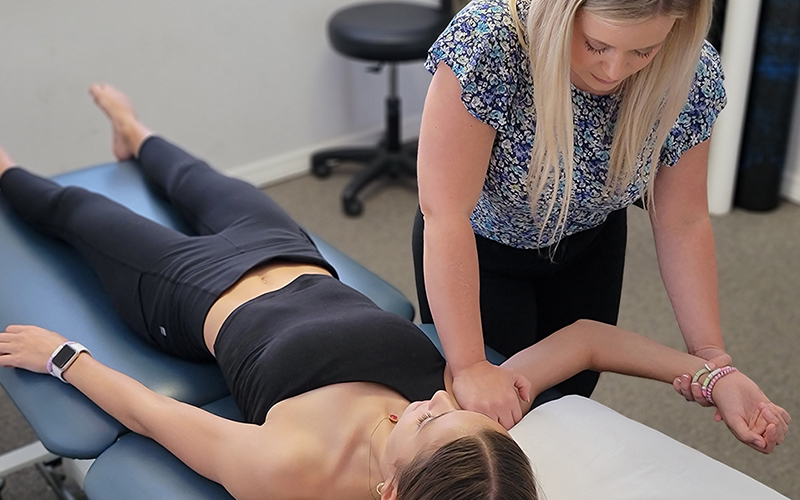
No waiting periods
Get off that waiting list and get the treatment you need. We're always ready to accept new patients, so you can get better faster and get back to a pain-free life that you deserve.
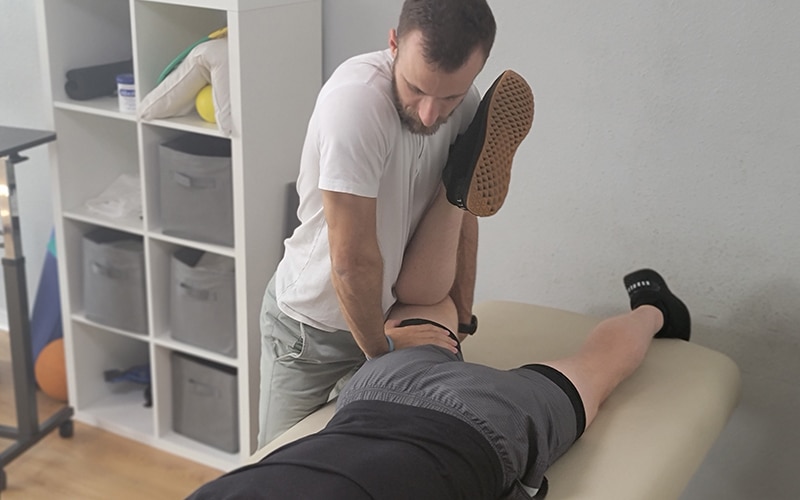
Not limited by insurance
Don't let the insurance companies tell you how much treatment you need. Avoid the limitations of short sessions that insurance provides and work with our Doctors when you need it and for as long as you need it.
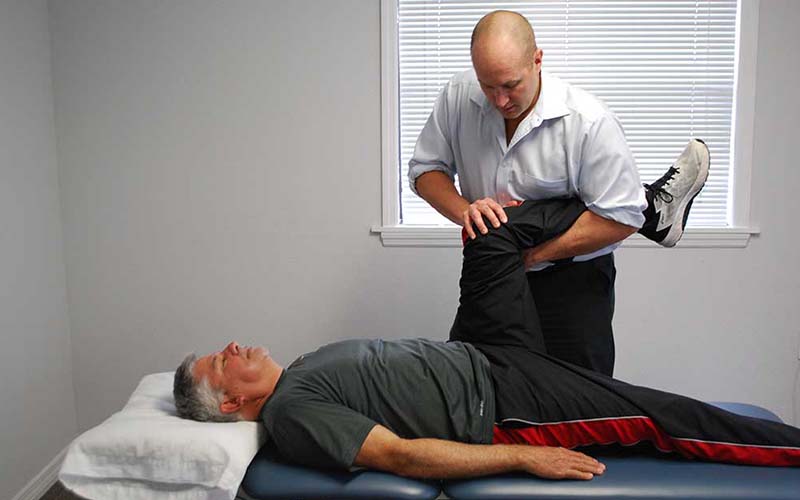
No painful injections, no expensive medications, no surgery
In order to truly solve your pain, we use a holistic approach to Physical Therapy, not relying on injections, medications, or surgery. Instead, we'll strengthen your body's weak points that are causing your pain.
MEET THE TEAM

RON MILLER, DPT, OCS, Cert DN
Doctor of Physical Therapy | Board Certified Orthopaedic Physical Therapy Clinical Specialist | Post-Doctoral Orthopaedic Residency Trained | Certified in Dry Needling | Titleist Performance Institute Certified
Dr. Ron Miller is the owner and founder of Pursuit Physical Therapy. His core belief is that it is not about the physician, the physical therapist, or the insurance company: it is about what is truly best for the patient. Dr. Miller started...

MARYANN DANIELS, PT, MCMT, IDN
Physical Therapist | Dry Needling Certified | Mastery Certified In Manual Therapy | Pelvic Floor And Post Partum Specialist
Maryann was originally born in Connecticut but moved to Florida with her family at the age of 9 and she grew up in Jupiter, Florida. She then went to college at the University of Central Florida...


MICHAEL FABRICK, DPT, Cert. DN
Doctor of Physical Therapy | Certified in Dry Needling | Pursuit Sports Performance Specialist | Professional Tennis Tour Physical Therapist
Dr. Michael Fabrick was born and raised in Hanover, Pennsylvania and attended Slippery Rock University where he received his Bachelor’s degree in Exercise Science. He then went on to receive his Doctorate Degree in Physical Therapy in May of 2020. During his final tenure as a Doctoral intern, he trained underneath Todd Ellenbecker...

THOMAS EBERLE, DPT, FAAOMPT
Doctor Of Physical Therapy | Fellow, American Academy Of Orthopedic Manual Physical Therapist | Dry Needling Certified |
Dr. Thomas Eberle is a native of Buffalo, New York where he completed his Master of Science, Physical Therapy from D’Youville College. Dr. Eberle went on and further completed his Doctor of Physical Therapy, an Orthopedic Residency, and a Fellowship program...


Will Deiss, DPT, CSCS
Doctor of Physical Therapy | Certified Strength & Conditioning Specialist
Dr. Will Deiss was born in Chicago, Illinois, but moved to Virginia as a toddler, where he was raised in Mechanicsville. He attended James Madison University (Go Dukes), where he received a Bachelor of Science in Kinesiology. He then completed his Doctor of Physical Therapy degree...
BECOMING PAINFREE IS EASIER THAN YOU THINK

Step 1:

Step 2:


 Charles D.
Charles D. Lisa B.
Lisa B.