Best Orlando Physical Therapy for
SCIATICA
Are you struggling to enjoy your favorite hobbies or daily activities due to sharp low back or sciatica pain? With the expertise of our specialized doctors, we can identify the root cause of your symptoms and provide effective treatment, helping you get back to what you love faster and with lasting relief.
Best Orlando Treatment for a
SCIATICA
Are you not able to continue your cherished hobbies or everyday activities because of sharp pain in your low back when you move? With our expert doctors’ help, you can get to the root of your symptoms and get back to doing what you love quicker and easier.
Read More Ask A QuestionHere Is Everything You Need To Know About Sciatica, What Causes It, and The Best Way to Treat It
Click the tabs below to get direct answers to your questions
What is sciatica?
It’s estimated that as many as 75% of us will have some form of back or neck pain at some point in our lifetime. The good news is that most of us will recover without the need for surgery—and conservative care such as physical therapy usually gets better results than surgery. A herniated disk is one cause of neck and back pain.
What are common causes of sciatica?
Your spine is made up of 33 vertebrae (bones) that are stacked on top of one another. Between each vertebra is a cushion-like piece of cartilage called an “intervertebral disk.” Imagine the disk as a tire, with gelatin filling the hole in the tire. The rubbery outer part is called the “annulus,” and the gelatin is called the “nucleus.” When we’re young—under 30 years of age—the disk is made mostly of gelatin. As we age, we start to lose some of that gelatin. The disk becomes flatter and less flexible, making it easier to injure. In some cases, the gelatin can push out through a crack in the rubbery exterior and lead to a herniation (bulge) or rupture (tear).
Herniated disks are most common in the neck (cervical spine) and low back (lumbar spine). In the low back, disks may become damaged by excessive wear and tear or an injury.
Your risk for developing a herniated disk increases due to:
- Age – most herniated discs occur in people who are 30 to 50 years of age as a result of age-related disk degeneration. Herniated disks are less common after the age of 50, however, because with aging there is less fluid to push out of the disk
- Obesity – increased weight results in increased pressure on the disks
- Occupation – jobs that are physically demanding and involve repetitive tasks such as lifting, pushing, pulling, and twisting place additional stress on the disks
- Low levels of physical activity – people who are not physically active are less able to handle physical demands
Where does it hurt?
In most cases of sciatica,
What are common symptoms of sciatica?
You might have mild to intense neck or back pain—or no pain at all. Herniated disks sometimes show up on the diagnostic images of people who have no symptoms.
When the disk ruptures (“herniates”) and a portion of the disk pushes outside its normal boundaries, it can “pinch” or press on spinal nerves or the spinal cord. This condition is called “radiculopathy.” The pressure can lead to back pain or to pain, numbness, or weakness in the legs.
The type and location of your symptoms depends on the location and the amount of pressure on the nerves:
- If you have a herniated disk in the cervical spine, you may have pain, tingling, numbness, weakness, or any combination of these symptoms in the arm, shoulder, or neck
- If you have a herniated disk in the lumbar spine, you may have pain, tingling, numbness, weakness, or any combination of these symptoms in the back, buttocks, or legs; most likely, your symptoms will be on only one side of your body
Often, symptoms from herniated disks are made worse by certain activities or positions. If you have a herniated disk in the lumbar spine:
- Pain may get worse with sitting, bending, and reaching
- Pain may be
worst first thing in the morning and after staying in one position for a long time - You may need to switch positions frequently
- You may prefer to stand rather than sit
If you have a herniated disk in the neck, symptoms are often worse with prolonged sitting and when lying down.
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, and It's Free!

- Learn The Essential First Step... So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results!
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, And It's Free!

- Learn The Essential First Step...So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
Can sciatica be treated?
Yes, sciatica can be treated and with great results. Even better, many times it can be treated conservatively without needing injections, pain medications, or surgeries if you can address it early enough. The key to treatment is to solve the root cause of your pain so you can get the best results and a long-term outcome.
Some root causes of sciatica pain can be:
- A decreased mid back range of motion
- Poor posture in sitting
- Lack of hip range of motion
- Weak hip and glute muscles
- Poor lifting biomechanics
- Overloading low back area
- Repeated bending forward at work
- Tight low back and hip joints
- Poor biomechanics at work
- Too much sitting
- Developing fear of pain and movement
If you have failed multiple treatment approaches already, your clinician missed the real root cause of your pain and was just chasing the symptoms. The pain or symptom is the effect, not the cause. What do I mean by this? Say your fire alarm goes off in your house. Its purpose is to protect you and make you aware that something is wrong, i.e., that there is a fire in your house. The “alarm” is like your pain (your body’s way of telling you something is wrong) and the “fire” is the root cause. When the fire alarm goes off, you don’t run upstairs and just turn it off, right? You run through the house with the fire extinguisher, trying to find the room where the fire is at. You try to find out what caused the alarm to go off so you can put it out. Once the fire is out, then the fire alarm can go off. Solve the “root” cause of your pain, and then the pain (“the effect”) eventually goes away.
Additionally, there is a common root cause which many clinicians misdiagnose. They treat the sciatica pain with a cookie cutter approach, hoping it will work and treat it as a simple muscle problem. They tend to rely on stretching, ultrasound, massage, and focus treatment directly on the low back area. However, often the root cause is missed and the symptoms return. If you have failed multiple low back treatments and still have low back pain, then maybe it’s not a low back problem? Hmmm. Maybe the root cause in the hips! So many healthcare clinicians treat pain like this and thus show poor treatment outcomes which results in the pain coming back. Why? They missed the root cause of your sciatica pain. This is also the case when patients turn to injections, nerve blocks and other surgeries which are still not effective because the actual problem still is not solved, their treatment was just chasing the pain.
The first step in treatment is to identify the root cause of your pain. A specific and individualized treatment approach for your type of pain can lead to a successful outcome for you and resolve your symptoms for the long term. This is why you can’t rely on a standard cookie cutter approach; you need a customized and individualized treatment approach specifically for your type of sciatica pain.
What happens if it goes untreated?
Minor case – If it is a minor case of sciatica, research shows that many acute cases of pain may spontaneously go away in 4-8 weeks. Many people say they have a herniated disc but this may be a false positive finding? Meaning it is not the cause of the low back pain and you had this before you started having low back pain? I have a herniated disc at L5-S1 and I don’t have sciatica! You still need to solve the root cause of your specific low back pain. But who wants to wait 8 weeks to get pain free? Let’s try to solve the root cause of your pain in 2-3 weeks and address all of the risk factors present (so it never returns!) and get you back to your favorite activities faster! We still recommend that you get it checked out by one of our board-certified physical therapists to ensure that it is just a minor case, to solve all risk factors, and to get the optimal outcome in the fewest visits needed. Most minor cases resolve on their own in time or get better with some stretching and strengthening. But, the sooner you take action, the sooner you are pain-free. (And research supports this!)
Severe case – If it’s more of a severe and chronic case of sciatica, your pain will probably start to worsen and increase because the root cause of the pain is not being treated. What is causing sciatica? Is it a herniated or is it stenosis and compression? Many people turn to pain medication and injections at this time but this only blocks the pain for short term. You may not feel the pain when taking pain medications, but the underlying problem is still there. Many people say after the pain medication is stopped, then usually the pain returns and sometimes it returns even worse. This is when you may experience chronic low back muscle pain, radiating pain into your buttock region and hip. Standing, walking, running, bending forward, lifting, and driving all increase your pain now and cause the pain to radiate into your buttocks and hip. If sciatica continues to worsen, you may start experiencing more radicular symptoms into your leg. You may have shooting leg pain, electrical like pain, and some numbness and tingling. At this point, the herniation, compression, and swelling around it may be getting worse and now it’s pinching on a nerve root, thus causing your radiating pain. You may even start experiencing numbness and tingling in the shin and foot. If you are getting more neurological symptoms like total numbness, drop foot, losing reflexes, muscle atrophy, this is an immediate medical emergency and you need to consult a specialist ASAP. Even though in many cases, it’s more chronic now, we can still help. Once the root cause is addressed, then we can start decreasing your pain, regardless of how chronic and severe the pain is. This is the crucial first step. It just may take more time to recover from a chronic case. Usually with chronic and severe cases, the longer you have your pain and injury, the longer it takes to resolve.
What outcome can you expect from treatment?
As we’ve discussed, the first step is to solve the root cause of your sciatica pain. This is the most essential step to plan a treatment specialized for you and your unique type of pain. Your root cause will guide your treatment and dictate what is the best way to treat your pain. This, along with identifying risk factors that may be predisposing you to have your pain and injury, will allow you to start getting pain free again. The next step is to start decreasing pain, modifying activities, and start addressing all of the impairments causing your pain which we discovered during your evaluation. With each session, pain should start to decrease and you should start to regain range of motion with less pain and symptoms. Any radicular and referred pain should resolve fast as well. At this point, we begin light and basic strengthening only if it does not increase pain. Treatment will consist of a lot of manual therapy and light exercises.
The next step is to achieve full range of motion, (which should correlate to being pain-free) and now we can start progressive strengthening. Strengthening the muscles is crucial and research shows that this gives you the best long-term outcome! As you start to get stronger and maintain your mobility, your pain will continue to decrease if it is not already gone. Your increased strength will allow you to perform more activities and prevent flare-ups. This usually does take up to 4 weeks. As you clear our goals, then we can start easing you back into sport, golf, running, and whatever your favorite activities are. This is when we start winding down treatments and getting you back into functional strengthening, sport specific training, return to run programs, golfing, and whatever your goals are. In the end, we reassess everything, making sure we achieved all of our goals, your goals, that all risk factors are gone, and finalize your long-term home exercise program. There are many factors which can influence your outcome, but 85-90% of our patients respond well to our treatment approach and achieve a successful outcome when completing their plan of care.
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, and It's Free!

- Learn The Essential First Step... So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results!
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, And It's Free!

- Learn The Essential First Step...So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
How is it diagnosed?
Your physical therapist will conduct a thorough evaluation that includes a review of your medical history and will use screening tools to determine the likelihood of a herniated disk. For example, the therapist will:
- Ask you very specific questions about the location and behavior of your pain, weakness, and other symptoms
- Ask you to fill out a body diagram to indicate specific areas of pain, numbness, and tingling
- Perform tests of muscle strength and sensation to determine the severity of the pressure on your nerves
- Examine your posture and observe how you walk and perform other activities
- Measure the range of motion of your spine and your arms and legs
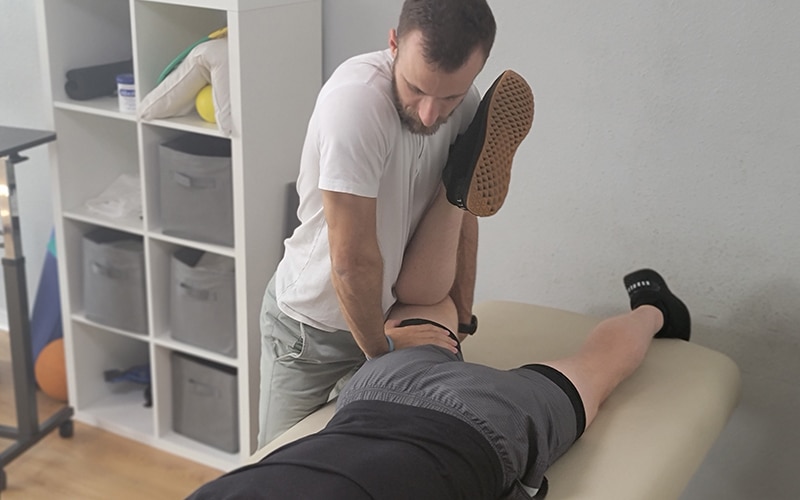
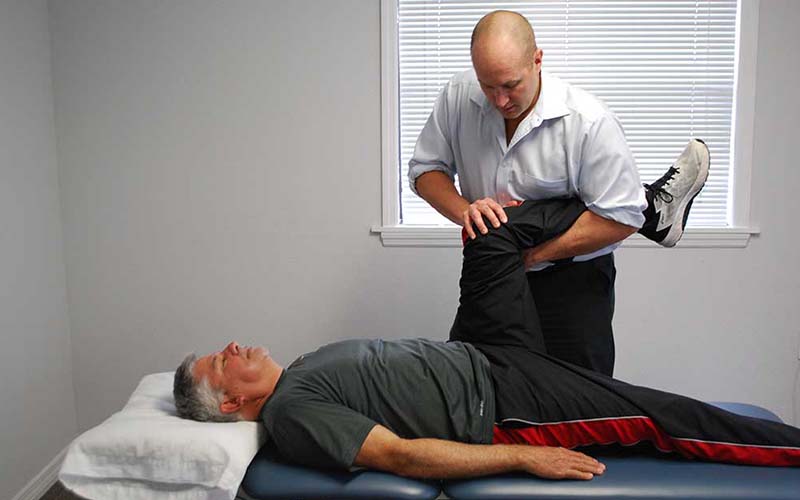
- Perform special tests, such as the straight leg raise test or the crossover straight leg raise test, that help diagnose a herniated disk
- Use manual therapy to evaluate the mobility of the joints and muscles in your spine
- Test the strength of important muscle groups
If you have muscle weakness and loss of sensation or very severe pain, special diagnostic tests, such as magnetic resonance imaging (MRI), electromyography, or nerve conduction studies may be needed. Physical therapists work closely with physicians and other health care providers to make certain that you receive an accurate diagnosis and appropriate treatment.
Research shows that in all but the most extreme cases (usually involving muscle weakness or high levels of pain), conservative care, such as physical therapy, has better results than surgery.
If your physical therapist’s evaluation indicates that there are no signs of nerve compression and you don’t have any signs of muscle weakness or numbness, treatment can begin right away. If the evaluation indicates that the herniated disk might be compressing the nerves, your therapist will consult with a physician specialist.
Do you need an X-ray and MRI imaging for sciatica pain?
For most common orthopedic cases, imaging is not needed and the diagnosis can be made with a simple physical therapy evaluation. No need to waste thousands of dollars on unwarranted diagnostic imaging. We also have clinical tests which we can perform to help rule in and rule out pathologies that correlate to MRI findings (which is WAY cheaper than an MRI!). An expensive MRI may just tell us what we already know. Also, often times the positive findings found on x-rays, MRIs, and EMGs may not actually be the root cause of your pain. What does that mean? Many positive findings on an MRI are also found in asymptomatic (pain-free) individuals, so diagnostic imaging may not be able to tell us what is actually causing your pain. For example: many people have a herniated disc in their low back but do not have any low back pain. So if herniated discs can cause no pain, just because someone with low back pain has a herniated disc does not mean that is what’s causing their pain. The key is to find out if your clinical evaluation findings during your evaluation at Pursuit match the MRI findings. If so, then we can decide what is the best way to treat it.
How can a Physical Therapist treat it?
Your physical therapist’s overall purpose is to help you continue to participate in your daily activities and life roles. The therapist will design a treatment program based on both the findings of the evaluation and your personal goals. Your treatment program most likely will include a combination of exercises.
Your therapist will design:
- Exercises that involve specific movements to relieve nerve pressure and decrease pain and other symptoms, especially during the early stages of treatment
- Stretching and flexibility exercises to improve mobility in the joints and the muscles of your spine, arms, and legs—improving motion in a joint can be key to pain relief
- Strengthening exercises—strong trunk muscles provide support for your spinal joints, and strong arm and leg muscles help take some of the workload off those joints
- Aerobic exercise, which has been proven to be helpful in relieving pain, promoting a healthy body weight, and improving overall strength and mobility—all important factors in managing a herniated disk
This might sound like a lot of exercise, but don’t worry: research shows that the more exercise you can handle, the quicker you’ll get rid of your pain and other symptoms.
Your physical therapist also might decide to use a combination of other treatments:
- Manual therapy to improve the mobility of stiff joints and tight muscles that may be contributing to your symptoms
- Posture and movement education to show you how to make small changes in how you sit, stand, bend, and lift—even in how you sleep—to help relieve your pain and help you manage your condition on your own
- Special pain treatments—such as ice, traction, and electrical stimulation—to reduce pain that is severe and not relieved by exercise or manual therapy
Once your pain is gone, it will be important for you to continue your new posture and movement habits to keep your back healthy.
How long does it take for recovery?
Recovery time for sciatica pain depends on multiple factors:
- The severity and chronicity of your pain
- Whether your pain is an easy or complex case
- If the root cause of your pain was solved or if it was missed (this is the key to getting a great recovery!)
- How long you have been in pain for and when you need to be pain-free by
- Other therapies and treatments you have tried
- Which medical professional(s) you saw prior to seeing us
- How active you are in trying to resolve your pain
- Which treatment approach is chosen and if it is proven to work for your pain
There are many factors that influence your recovery time and every patient’s recovery time is different. If you do nothing and don’t pursue treatment, it could gradually get better on its own, you could continue to have the same pain persist, or it could continue to get worse. As stated earlier, most acute cases may or may not resolve in 4-8 weeks. If you get expert treatment that solves the root cause of your pain, some cases resolve in 1-3 weeks! Then you can get back to sports, exercise, and your favorite activities without flare-ups and recurrences. Some of our patients are pain-free in 1-3 visits and back to 100% in 2 weeks!
If it is a complex case with chronic pain, your recovery may take longer, but you can still get a good outcome. Some chronic cases can resolve as fast as 2 months but can take as long as 4-6 months. It varies with every patient because every case of sciatica pain is different. Every patient’s recovery varies depending on the factors listed above. After a thorough evaluation here at Pursuit Physical Therapy, you will know your exact timeline of recovery, your prognosis, and when you should reach your goals.
How much does it cost?
The average cost of care for a case of spine pain in the US is $1800-$6600. This high price is due to many factors: the over-inflated cost of healthcare, the over expensive cost of unwarranted imaging (x-rays, CT scans, and MRIs) that is not needed, over-utilization of care (which increases the number of visits needed to be treated, requiring multiple visits to different doctors and physical therapists for the same diagnosis), and getting billed for unnecessary and unproven treatments that you don’t even need. All of these factors increase cost and this is why healthcare is so expensive. We strive to end that unnecessary, expensive cycle. In fact, we are currently publishing our first-year data with the University of Central Florida that shows the cost-effectiveness of our treatment approach.
This year, the average cost of our care was shown to be $814-$1141. Some of our patients get even as low as $315 for the full treatment! So if you have a deductible of $3,000-$10,000 and you have to pay out of pocket for your treatment, we can save you lots of money.
Remember, every case of pain is different and not all sciatica pain is the same. It is hard to predict exactly how much your treatment is going to cost you. But after a thorough evaluation, we can tell you exactly what is causing your pain, how long it is going to take, what the best way to treat it will be, and exactly how much it is going to cost. We have no hidden fees, no co-pays, and no miscellaneous bills that you will be surprised by 3 months after you receive treatment. Your pain, your diagnosis, your goals, and what is best for you dictate your treatment and how much it will cost, and while it varies for every patient, treatment at Pursuit is still much more affordable than standard healthcare.
How long are sessions?
Our evaluations are always one-on-one with one of our board-certified specialists and 60-90 minutes long. We like to perform thorough evaluations so we can solve the root cause of your pain, identify all risk factors, and make sure that we do it right. After the evaluation, you will know your diagnosis, the root cause of why you have your pain and symptoms, your prognosis, an expected timeline of when you should see results, what the best way to treat your pain is, how much it will cost, and your expected recovery outcome. We want you to fully understand everything about your pain and injury. What is best for you and will get you the best outcome is what will dictate your care and treatment. There will be plenty of time for you to ask questions so we can make sure you fully understand why you have your pain and what the best way to treat it will be. After the evaluation is completed, all treatment sessions are 60 minutes going forward and still one-on-one with your physical therapist. You and your physical therapist will design a customized treatment plan that works for you and that will achieve your goals
What are the next steps?
Getting started is simple. The first step, and the key to getting you
Solve the root cause of your pain
How Our Treatment is Different
We believe that working with a specific specialist for your care is the best way to solve the root cause of your pain. Work one-on-one with a Doctor of Physical Therapy every time your visit our office.
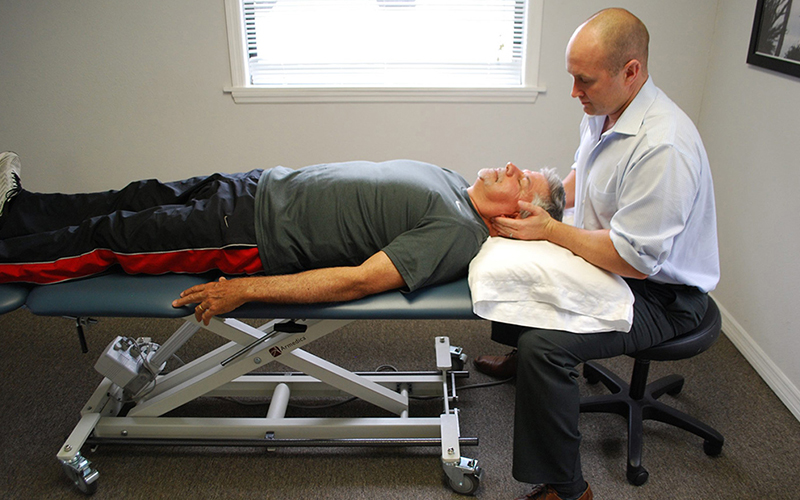
Exclusive one-on-one patient care
While most clinics will give you a limited amount of time with your Doctor, we believe that true results come from consistent one-on-one therapy.
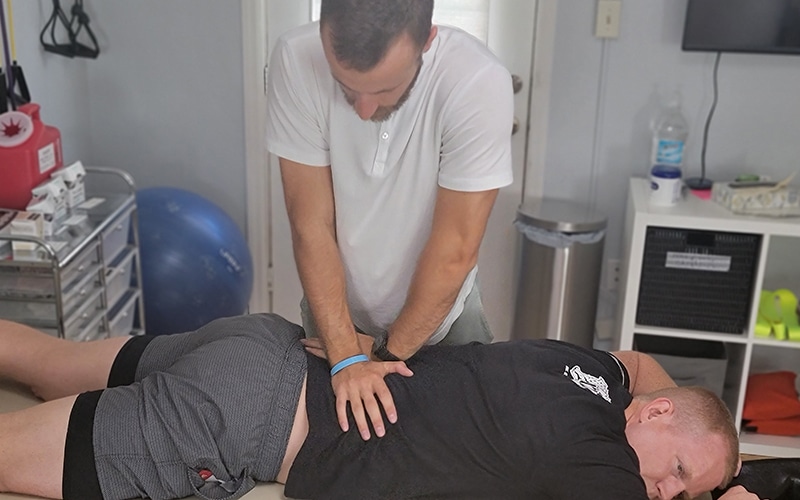
Work with your specialist every visit
Stop being handed off to trainees or non-Doctors for your Physical Therapy. At Pursuit, you'll work exclusively with your Doctor of Physical Therapy that specializes in your specific needs.
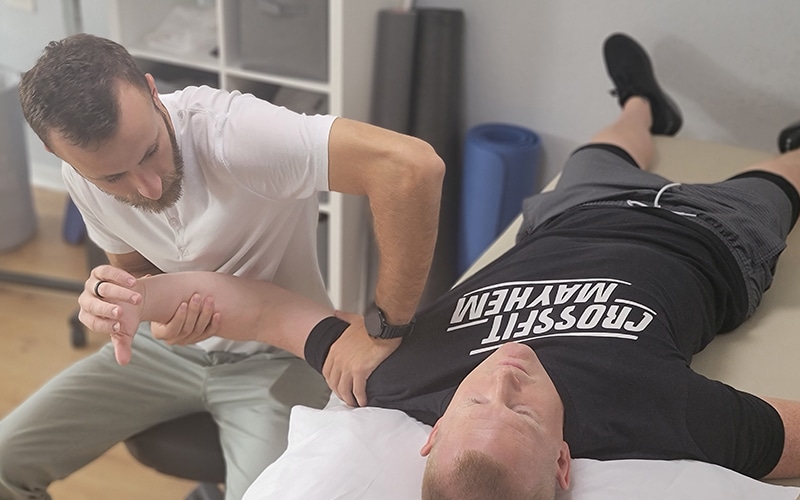
24/7 messaging access to your specialist
Ever have an issue or questions? We're here to help. Get 24/7 access to your specialist while you're under our care. Physical Therapy doesn't just happen when you're in our clinic, so we're here for you when you need us.
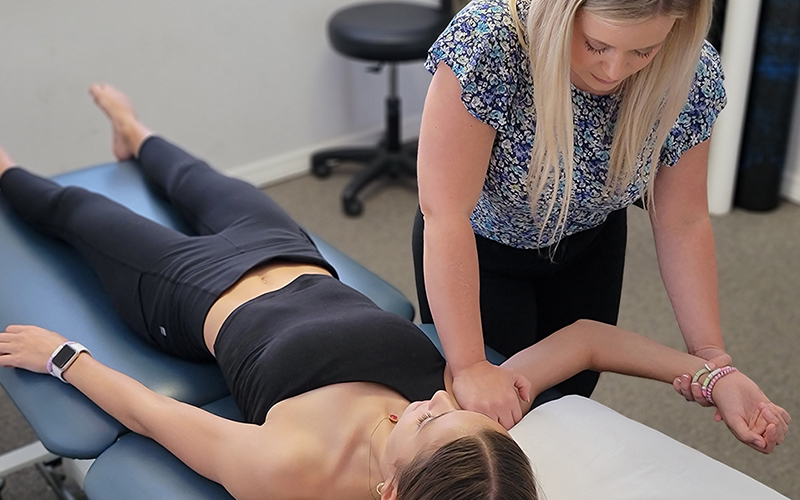
No waiting periods
Get off that waiting list and get the treatment you need. We're always ready to accept new patients, so you can get better faster and get back to a pain-free life that you deserve.
Not limited by insurance
Don't let the insurance companies tell you how much treatment you need. Avoid the limitations of short sessions that insurance provides and work with our Doctors when you need it and for as long as you need it.
No painful injections, no expensive medications, no surgery
In order to truly solve your pain, we use a holistic approach to Physical Therapy, not relying on injections, medications, or surgery. Instead, we'll strengthen your body's weak points that are causing your pain.
MEET THE TEAM

RON MILLER, DPT, OCS, Cert DN
Doctor of Physical Therapy | Board Certified Orthopaedic Physical Therapy Clinical Specialist | Post-Doctoral Orthopaedic Residency Trained | Certified in Dry Needling | Titleist Performance Institute Certified
Dr. Ron Miller is the owner and founder of Pursuit Physical Therapy. His core belief is that it is not about the physician, the physical therapist, or the insurance company: it is about what is truly best for the patient. Dr. Miller started...

MARYANN DANIELS, PT, MCMT, IDN
Physical Therapist | Dry Needling Certified | Mastery Certified In Manual Therapy | Pelvic Floor And Post Partum Specialist
Maryann was originally born in Connecticut but moved to Florida with her family at the age of 9 and she grew up in Jupiter, Florida. She then went to college at the University of Central Florida...


MICHAEL FABRICK, DPT, Cert. DN
Doctor of Physical Therapy | Certified in Dry Needling | Pursuit Sports Performance Specialist | Professional Tennis Tour Physical Therapist
Dr. Michael Fabrick was born and raised in Hanover, Pennsylvania and attended Slippery Rock University where he received his Bachelor’s degree in Exercise Science. He then went on to receive his Doctorate Degree in Physical Therapy in May of 2020. During his final tenure as a Doctoral intern, he trained underneath Todd Ellenbecker, who is one of the world’s leading experts on shoulder rehabilitation and is the Vice President of Medical Services for the ATP World Tour...

THOMAS EBERLE, DPT, FAAOMPT
Doctor Of Physical Therapy | Fellow, American Academy Of Orthopedic Manual Physical Therapist | Dry Needling Certified |
Dr. Thomas Eberle is a native of Buffalo, New York where he completed his Master of Science, Physical Therapy from D’Youville College. Dr. Eberle went on and further completed his Doctor of Physical Therapy, an Orthopedic Residency, and a Fellowship program...

BECOMING PAINFREE IS EASIER THAN YOU THINK

Step 1:

Step 2:


 Jackie M.
Jackie M. Lisa B.
Lisa B.