Shoulder Joint Pain
- No painful injections
- No unnecessary surgery
- No expensive medications
Shoulder Joint Pain
- No painful injections
- No unnecessary surgery
- No expensive medications
What is Osteoarthritis of the Shoulder?
Shoulder osteoarthritis (OA) occurs when the cartilage that lines the opposite sides of the shoulder joint becomes worn or torn. In the early stages of the condition, small pits develop in the smooth cartilage that lines each side of the joint. Eventually, small protrusions of bone, or “bone spurs” develop at the edges of the joint surfaces. Joint fluid may also accumulate under the cartilage, forming cysts, which can put pressure on the bone and may contribute to pain. In the late stages of the condition, the cartilage can wear away completely, allowing bone-to-bone contact. Two bones make up the shoulder joint. The bone at the top of the arm, the humerus, has a round, ball-shaped head, covered in cartilage. The bone on the body side of the joint is the scapula, or shoulder blade. The flat, cartilage-covered surface on the scapula that makes the other half of the shoulder joint is called the glenoid. The 2 sides of the shoulder joint are surrounded and connected by ligaments that control motion in the joint. The ligaments at the front of the shoulder become tightened as OA progresses. In addition, the four main muscles that surround the shoulder, known as the rotator cuff, may be over-used, weaken, or even tear. Rotator cuff conditions occur in about 90% of people with shoulder OA.How Does Arthritis in the Shoulder Feel?
Shoulder OA may cause you to experience:- Pain with activities that relieves with rest
- Decreased shoulder movement (range of motion), especially when reaching back as if grabbing a seat belt
- Weakness
- Stiffness and eventual difficulty using the affected arm
- Pain at rest and difficulty sleeping as the condition worsens
How Is Arthritis in the Shoulder Diagnosed?
Your doctor may order an x-ray to determine the amount of change in the joint. As the cartilage wears down, it decreases the space between the bones visible on these images. Bone spurs or cysts may also be present. Apparent damage often does not directly correlate with your pain. If there is suspected loss of bone, a CAT scan (computerized topography) may be ordered to get a clearer picture of the area. Your physical therapist will ask questions about how the shoulder problem is affecting your life, and what activities are now difficult for you. Describing your pain will help determine the best plan for your treatment. Your physical therapist will evaluate how far the shoulder can move, both as you move your arm and as he or she moves it for you. The examination will include evaluating the strength of the muscles of the rotator cuff and those that support the shoulder blade. The physical therapist may look at your posture and how you perform certain activities and movements to see how they affect your shoulder.Without Surgery
When someone develops shoulder pain, the first recommended treatment is physical therapy. The following treatments can help decrease pain, improve movement, and allow increased use of your shoulder for daily activities. They may prolong the time until surgery is needed, or help you avoid it altogether.- Improving tolerance of daily activities. Your physical therapist will work with you to help you get back to performing your daily tasks. Just changing your posture can reduce the pressure and forces at the joint and help reduce your pain. He or she may recommend the use of physical therapy “modalities” such as heat and cold, teach you about proper movement, and help you modify your activities to control your pain.
- Improving shoulder mobility. Your physical therapist can recommend ways to restore shoulder movement (range of motion). Stretching can lengthen tight muscles and ligaments, improving your posture and movement. Shoulder-joint mobilization may help improve movement and ease your pain. Your physical therapist may gently move your shoulder (manual therapy), to stretch the ligaments in ways normal stretching or arm motions do not.
- Improving the strength of your muscles. Strengthening the rotator cuff muscles can reduce the friction caused by the rough arthritic surfaces of the shoulder joint rubbing together. Support from the muscles that maintain your posture can help reduce forces on the shoulder joint.
Following Surgery
There are several surgical options for treating shoulder OA, depending on the degree of damage at the joint and its surrounding structures, and your age, activity level, and occupation. Palliative Options: The goal of this surgery is to resolve symptoms; it does not restore or reconstruct the arthritic area. This option is best for people under the age of 65 with minimal cartilage problems, or people in their 20s to 40s with many active years ahead. Reparative, Restorative, and Reconstructive Options: Over the last several years, surgeons have developed new “biologic resurfacing” techniques for younger people who have shoulder OA who are not yet ready for total shoulder replacement. Your doctor and physical therapist can describe them in detail for you. Total Shoulder Arthroplasty (TSA): Total shoulder arthroplasty is the medical term for a shoulder replacement. This is the best surgical technique for older patients with advanced OA who have good quality of bone at the shoulder joint and intact rotator cuff muscles. This procedure is best for people who do not plan to do high-level activities (overhead work at a job, overhead sports, or significant amounts of heavy lifting). Shoulder Hemiarthroplasty: Shoulder hemiarthroplasty is a partial replacement of the joint. It is an option if the muscles that make up the rotator cuff of the shoulder are too weak or damaged to properly support and move the joint.Reverse (Inverse) Total Shoulder Arthroplasty (rTSA): This surgery is also an option when the muscles that make up the rotator cuff of the shoulder have failed or are irreparable, or a complex fracture is present.
Arthroscopy: Many shoulder surgeries can be done via arthroscopy, a less invasive surgery by which the surgeon makes small incisions in the skin and inserts pencil-sized instruments (with a camera) into the joint to repair damage. Postsurgical physical therapy varies based on the procedure performed. It may include:- Ensuring your safety as you heal. Your surgeon and physical therapist work together as a team to return your shoulder to health. After the surgeon completes his or her work, your work begins. You will perform specific activities and exercises at the correct time to allow for optimal healing. All surgical procedures modify your shoulder joint and surrounding tissues. Restorative and reconstructive options may take several months to heal, with longer precautions.
- Aiding motion of the shoulder. After surgery, your shoulder will be sore and swollen, and you may not feel like moving your arm. However, gentle motion is often recommended. Your physical therapist may move your arm or assist you in moving your arm to begin to gently restore movement. After some surgeries, movement is restricted during healing; your physical therapist and surgeon will choose the best options for recovery and guide you through the process.
- Strengthening the shoulder. Due to prior disuse or postoperative pain, your muscles may not be as strong as normal. If the muscle was repaired during surgery, you will have to let it heal for a period of time, and your physical therapist can let you know what activity is safe to help the healing along.
- Relieving your pain. Using manual (hands-on) therapies and other modalities, your physical therapist can help reduce your pain during exercise and daily activities.
- Getting back to work and activities of daily living. Returning to work and daily activities may be slow, and your physical therapist will guide you through the process to achieve the best results.
Can Arthritis in the Shoulder be Prevented?
There is no way to prevent shoulder OA. You may reduce your risk by staying moderately active, keeping the shoulder strong, and keeping the shoulder muscles the appropriate length with stretching. Your physical therapist can help you determine what exercises will keep your shoulder healthy. Eating healthy and exercising will help you manage a healthy weight and healthy joints. Avoiding injuries to the shoulder joint will help reduce your risk of OA as well. References: http://www.moveforwardpt.com/SymptomsConditionsDetail.aspx?cid=16b4f971-66e1-4112-9f02-fe12292f07be#.VYrn9_lVikoTo Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, and It's Free!

- Learn The Essential First Step... So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results!
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
Solve the root cause of your pain
How Our Treatment is Different
We believe that working with a specific specialist for your care is the best way to solve the root cause of your pain. Work one-on-one with a Doctor of Physical Therapy every time your visit our office.
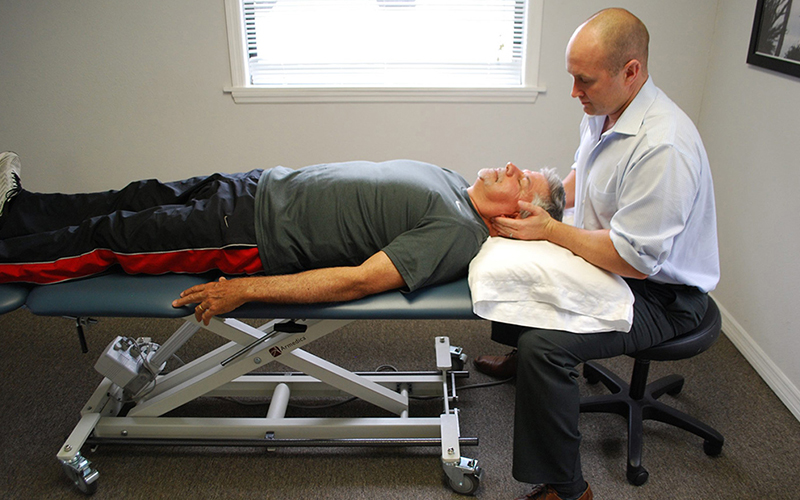
Exclusive one-on-one patient care
While most clinics will give you a limited amount of time with your Doctor, we believe that true results come from consistent one-on-one therapy.
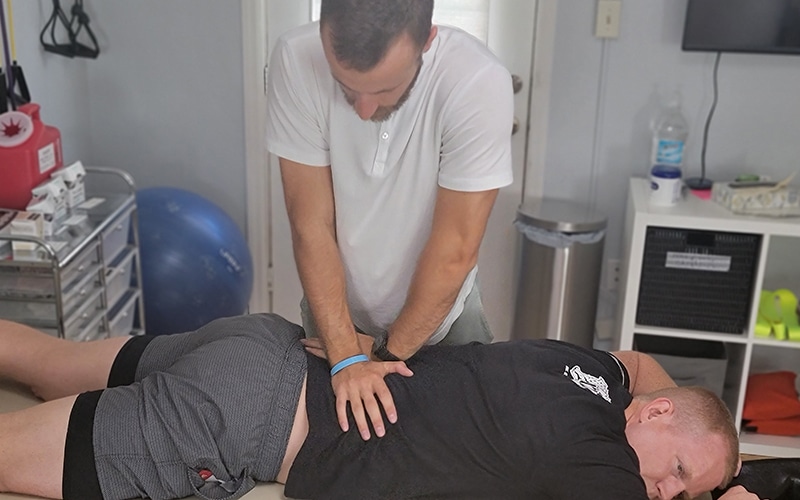
Work with your specialist every visit
Stop being handed off to trainees or non-Doctors for your Physical Therapy. At Pursuit, you'll work exclusively with your Doctor of Physical Therapy that specializes in your specific needs.
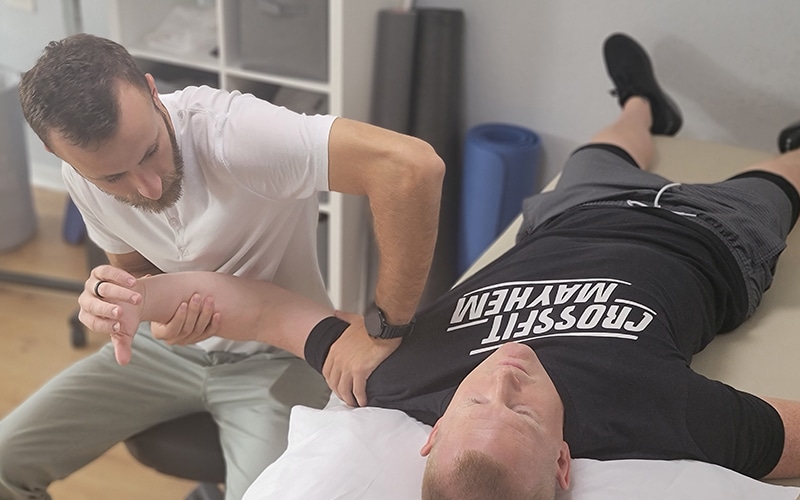
24/7 messaging access to your specialist
Ever have an issue or questions? We're here to help. Get 24/7 access to your specialist while you're under our care. Physical Therapy doesn't just happen when you're in our clinic, so we're here for you when you need us.
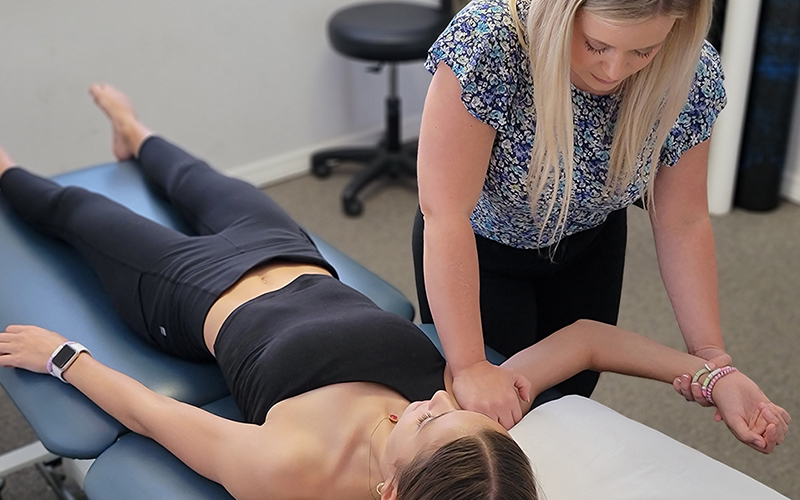
No waiting periods
Get off that waiting list and get the treatment you need. We're always ready to accept new patients, so you can get better faster and get back to a pain-free life that you deserve.
Not limited by insurance
Don't let the insurance companies tell you how much treatment you need. Avoid the limitations of short sessions that insurance provides and work with our Doctors when you need it and for as long as you need it.
No painful injections, no expensive medications, no surgery
In order to truly solve your pain, we use a holistic approach to Physical Therapy, not relying on injections, medications, or surgery. Instead, we'll strengthen your body's weak points that are causing your pain.
MEET THE TEAM

RON MILLER, DPT, OCS, Cert DN
Doctor of Physical Therapy | Board Certified Orthopaedic Physical Therapy Clinical Specialist | Post-Doctoral Orthopaedic Residency Trained | Certified in Dry Needling | Titleist Performance Institute Certified
Dr. Ron Miller is the owner and founder of Pursuit Physical Therapy. His core belief is that it is not about the physician, the physical therapist, or the insurance company: it is about what is truly best for the patient. Dr. Miller started...

MARYANN DANIELS, PT, MCMT, IDN
Physical Therapist | Dry Needling Certified | Mastery Certified In Manual Therapy | Pelvic Floor And Post Partum Specialist
Maryann was originally born in Connecticut but moved to Florida with her family at the age of 9 and she grew up in Jupiter, Florida. She then went to college at the University of Central Florida...


MICHAEL FABRICK, DPT, Cert. DN
Doctor of Physical Therapy | Certified in Dry Needling | Pursuit Sports Performance Specialist | Professional Tennis Tour Physical Therapist
Dr. Michael Fabrick was born and raised in Hanover, Pennsylvania and attended Slippery Rock University where he received his Bachelor’s degree in Exercise Science. He then went on to receive his Doctorate Degree in Physical Therapy in May of 2020. During his final tenure as a Doctoral intern, he trained underneath Todd Ellenbecker, who is one of the world’s leading experts on shoulder rehabilitation and is the Vice President of Medical Services for the ATP World Tour...

THOMAS EBERLE, DPT, FAAOMPT
Doctor Of Physical Therapy | Fellow, American Academy Of Orthopedic Manual Physical Therapist | Dry Needling Certified |
Dr. Thomas Eberle is a native of Buffalo, New York where he completed his Master of Science, Physical Therapy from D’Youville College. Dr. Eberle went on and further completed his Doctor of Physical Therapy, an Orthopedic Residency, and a Fellowship program...

To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, And It's Free!

- Learn The Essential First Step...So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
BECOMING PAINFREE IS EASIER THAN YOU THINK

Step 1:
Call our expert team.

Step 2:
We’ll work with you to find and treat the root of your pain.

Step 3:
Get back to doing what you love.
