Best Orlando Treatment for a
Heel Pain
Are you not able to continue your cherished hobbies or everyday activities because of Heel Pain when you move? With our expert doctors’ help, you can get to the root of your symptoms and get back to doing what you love quicker and easier.
Best Orlando Treatment for a
Heel Pain
Are you not able to continue your cherished hobbies or everyday activities because of Heel Pain when you move? With our expert doctors’ help, you can get to the root of your symptoms and get back to doing what you love quicker and easier.
Here Is Everything You Need To Know About Heel Pain, What Causes It, and The Best Way to Treat It
Click the tabs below to get direct answers to your questions
What is Heel Pain?
Iliotibial band syndrome (ITBS) is one of the most common causes of knee pain, particularly in individuals involved in endurance sports. It accounts for up to 12% of running injuries and up to 24% of cycling injuries. ITBS is typically managed conservatively through physical therapy and temporary activity modification.
What are common causes of Heel Pain?
Iliotibial band syndrome (ITBS) occurs when excessive irritation causes pain at the outside (or lateral) part of the knee. The iliotibial band (ITB) is a type of soft tissue that runs along the side of the thigh from the pelvis to the knee. As it approaches the knee, its shape thickens as it crosses a prominent area of the thigh (femur) bone, called the lateral femoral condyle. Near the pelvis, it attaches to 2 important hip muscles, the tensor fascia
Irritation and inflammation arise from friction between the ITB and underlying structures when an individual moves through repetitive straightening (extension) and bending (flexion) of the knee. Typically, ITBS pain occurs with overuse during activities such as running and cycling.
ITBS involves many lower extremity structures, including muscles, bones, and other soft tissues.
- Abnormal contact between the ITB and thigh (femur) bone
- Poor alignment and/or muscular control of the lower body
- Prolonged pinching (compression) or rubbing (shearing) forces during repetitive activities
The common structures involved in IT Band Syndrome are:
- Iliotibial band
- Bursa (fluid-filled sack that sits between bones and soft tissues to limit friction)
- Hip muscles
IT Band Syndrome can occur in:
- Athletes performing repetitive activities, such as squatting, and endurance sports such as running and cycling
- Individuals who spend long periods of time in prolonged positions, such as sitting or standing for a long workday, climbing or squatting, or kneeling
- Individuals who quickly start a new exercise regimen without proper warm-up or preparation
Where does it hurt?
Heel pain injuries occur anywhere along the bottom of the foot. In most cases, patients complain of pain on the bottom of the heel, the plantar fascia, or just around the heel bone. Some complex cases can experience pain at the specific attachment of the plantar fascia on the heel. This is real plantar fasciitis. Understanding the root cause of your pain is fundamental to treating your pain in the long run & will decrease your dependence on painkillers or treatment that only addresses the symptoms.
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, and It's Free!

- Learn The Essential First Step... So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results!
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, And It's Free!

- Learn The Essential First Step...So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
Can IT band syndrome be treated?
Yes, heel pain can be treated and with great results. Even better, many times it can be treated conservatively without needing injections, pain medications, or surgeries if you can address it early enough. The key to treatment is to solve the root cause of your pain so you can get the best results and a long term outcome.
Some root causes of heel
- Decreased ankle range of motion
- Poor running form
- Lack of ankle flexibility
- Weak hip and glute muscles
- Overload in training
- Poor lifting and running biomechanics
- Neural tension
- Leg length discrepancy
- Previous leg or hip injury
- Calf muscle weakness
- Poor footwear or running shoes
- Poor biomechanics with sports
- Trigger points in calf muscles
- Lack of foot range of motion
If you have failed multiple treatment approaches already, your clinician missed the real root cause of your pain and was just chasing the symptoms. The pain or symptom is the effect, not the cause. What do I mean by this? Say your fire alarm goes off in your house. Its purpose is to protect you and make you aware that something is wrong, i.e., that there is a fire in your house. The “alarm” is like your pain (your body’s way of telling
Additionally, there is a common root cause which many clinicians misdiagnose. They treat the foot pain with a cookie cutter approach, hoping it will
The first step in treatment is to identify the root cause of your pain. A specific and individualized treatment approach for your type of pain can lead to a successful outcome for you and resolve your symptoms for the long term. This is why you can’t rely on a standard cookie cutter approach; you need a customized and individualized treatment approach specifically for your type of heel pain.
What happens if it goes untreated?
Minor case – If it is a minor case of heel pain, research shows that many acute cases of pain may spontaneously go away in 4-8 weeks. The key to prevent from becoming a more severe chronic case is to solve the root cause of the
Severe case – If it’s more of a severe and chronic case of heel pain, your pain will probably start to worsen and increase because the root cause and underlying risk factors of the pain are not being treated. Many people turn to pain medication and injections at this time but this only blocks the pain for short term. You may not feel the pain when taking pain medications, but the underlying problem is still there. Many people say after the pain medication and injection wears off, then usually the pain returns and sometimes it returns even worse. This is when you cannot run, jump, or play sports. Once the root cause is addressed, then we can start decreasing your pain, regardless of how chronic and severe the pain is. This is the crucial first step. It just may take more time to recover from a chronic case. Usually with chronic and severe cases, the longer you have your pain and injury, the longer it takes to resolve.
What outcome can you expect from treatment?
As we’ve discussed, the first step is to solve the root cause of your heel pain. This is the most essential step to plan a treatment specialized for you and your unique type of pain. Your root cause will guide your treatment and dictate what is the best way to treat your pain. This, along with identifying risk factors that may be predisposing you to have your pain and injury, will allow you to start getting pain free again. The next step is to start decreasing pain, modifying activities, and start addressing all of the impairments causing your pain which we discovered during your evaluation. With each session, pain should start to decrease and you should start to regain range of motion with less pain and symptoms. Any radicular and referred pain should resolve fast as well. At this point, we begin light and basic strengthening only if it does not increase pain. Treatment will consist
The next step is to achieve full range of motion, (which should correlate to being
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, and It's Free!

- Learn The Essential First Step... So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results!
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
To Get A "Insider's Look" At Our Treatment Approach And How We Get Results...
Click Below To Watch Our Exclusive Webinar! It's Simple, Short, And It's Free!

- Learn The Essential First Step...So You Can Get Pain Free Again
- See Why Treatment Needs To Be Individualized, Not Standardized...So You Get Faster Results
- Learn How You Can Save Money...So You Don't Have To Waste $1000's On Unnecessary Treatments
How is it diagnosed?
When you seek help for heel pain, we will perform a comprehensive evaluation and ask questions about your pain and your daily activities.
These may include:
- How and when the pain started: Did the pain begin spontaneously or was there any trauma or injury experienced in the area?
- Where are the symptoms located, and have they changed location or intensity since the onset?
- What things make the symptoms better or worse?
- What type of work do you perform?
- What hobbies or household activities do you regularly perform?
- What is the worst your pain gets throughout the day?
- What activities throughout your day make your pain worse?
One of our board-certified physical therapists will perform a thorough assessment of your evaluation, testing: movement, a range of motion, joint mobility, strength, muscle activation, nerves, and functional movement. The therapist will also check your reflexes, do a medical screening (to rule out medical red flags and serious pathologies), and conduct special tests on your primary area of pain to determine what specifically may be involved and to rule out other conditions. The key to getting an accurate and correct diagnosis is a reproduction of your pain during the evaluation. We want to find out if we change (or even decrease) your pain during the evaluation. This is the key! To provide a definitive diagnosis, your therapist may also collaborate with an orthopedist or other healthcare providers. The orthopedist may order further tests, such as magnetic resonance imaging (MRI) or electromyography (EMG) if medical red flags are present. After the evaluation, you will know exactly what your diagnosis is and what exactly is causing your pain. You will have plenty of time to ask questions to ensure that you fully understand what is going on. The next step, then, is to determine what is the best way to treat it.
Do you need X-ray and MRI imaging for IT Band Syndrome pain?
For most common orthopedic cases, imaging is not needed and the diagnosis can be made with a simple physical therapy evaluation. No need to waste thousands of dollars on unwarranted diagnostic imaging. We also have clinical tests which we can perform to help rule in and rule out pathologies that correlate to MRI findings (which is WAY cheaper than an MRI!). An expensive MRI may just tell us what we already know. Also, often times the positive findings found on x-rays, MRIs, and EMGs may not actually be the root cause of your pain. What does that mean? Many positive findings on an MRI are also found in asymptomatic (pain-free) individuals, so diagnostic imaging may not be able to tell us what is actually causing your pain. For example, many people have a herniated disc in their low back but do not have any low back pain. So if herniated discs can cause no pain, just because someone with low back pain has a herniated disc does not mean that is what’s causing their pain. The key is to find out if your clinical evaluation findings during your evaluation at Pursuit match the MRI findings. If so, then we can decide what is the best way to treat it.
How can a Physical Therapist treat it?
Your physical therapist will use treatment strategies to focus on:
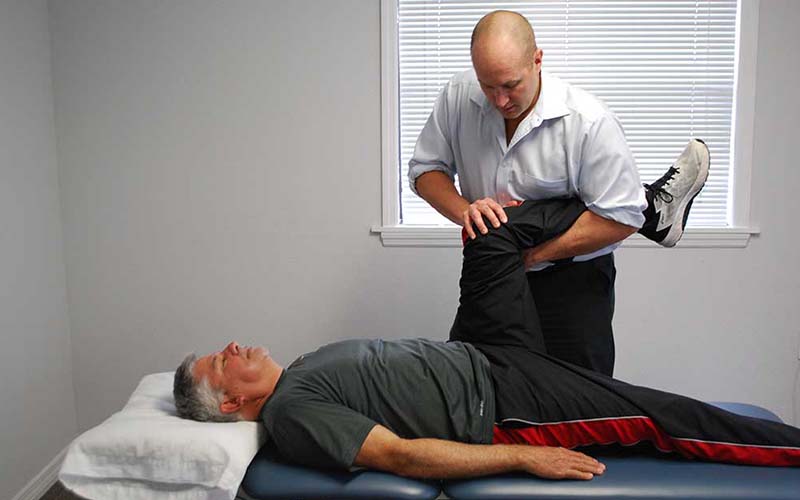
Range of motion
Often, abnormal motion of the hip and knee and foot joint can cause ITBS because of how the band attaches to hip muscles. Your therapist will assess the motion of your
Muscle strength
Hip and core weakness can contribute to ITBS. The “core” refers to the muscles of the abdomen, low back, and pelvis. Core strength is important, as a strong midsection will allow greater stability through the body as the arms and legs go through various motions. For athletes performing endurance sports, it is important to have a strong core to stabilize the hip and knee joints during repetitive leg motions. Your physical therapist will be able to determine which muscles are weak and provide specific exercises to target these areas.
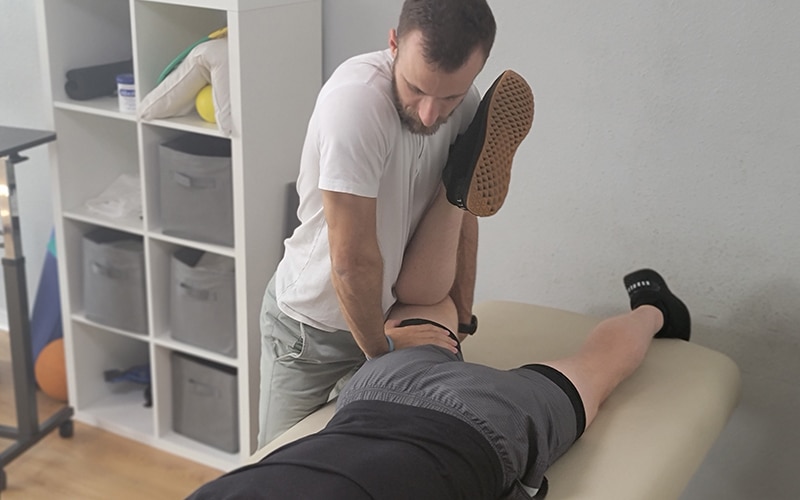
Manual therapy
Many physical therapists are trained in manual therapy, which means they use their hands to move and manipulate muscles and joints to improve motion and strength. These techniques can target areas that are difficult to treat on your own.
Functional training
Even when an individual has normal motion and strength, it is important to teach the body how to perform controlled and coordinated movements so there is no longer excessive stress at the previously injured structures. Your physical therapist will develop a functional training program specific to your desired activity. This means creating exercises that will replicate your activities and challenge your body to learn the correct way to move.
Your physical therapist will also work with you to develop an individualized treatment program specific to your personal goals. He or she will offer tips to help you prevent your injury from reoccurring.
How long does it take for recovery?
Recovery time for heel pain depends on multiple factors:
- The severity and chronicity of your pain
- Whether your pain is an easy or complex case
- If the root cause of your pain was solved or if it was missed (this is the key to getting a great recovery!)
- How long you have been in pain for and when you need to be pain-free by
- Other therapies and treatments you have tried
- Which medical professional(s) you saw prior to seeing us
- How active you are in trying to resolve your pain
- Which treatment approach is chosen and if it is proven to work for your pain
There are many factors that influence your recovery time and every patient’s recovery time is different. If you do nothing and don’t pursue treatment, it could gradually get better on its own, you could continue to have the same pain persist, or it could continue to get worse. As stated earlier, most acute cases may or may not resolve in 4-8 weeks. If you get expert treatment that solves the root cause of your pain, some cases resolve in 1-3 weeks! Then you can get back to sports, exercise, and your favorite activities without flare-ups and recurrences. Some of our patients are pain-free in 1-3 visits and back to 100% in 2 weeks!
If it is a complex case with chronic pain, your recovery may take longer, but you can still get a good outcome. Some chronic cases can resolve as fast as 2 months but can take as long as 4-6 months. It varies with every patient because every case of Achilles tendinopathy pain is different. Every patient’s recovery varies depending on the factors listed above. After a thorough evaluation here at Pursuit Physical Therapy, you will know your exact timeline of recovery, your prognosis, and when you should reach your goals.
How much does it cost?
The average cost of care for a case of spine pain in the US is $1800-$6600. This high price is due to many factors: the over-inflated cost of healthcare, the over expensive cost of unwarranted imaging (x-rays, CT scans, and MRIs) that is not needed, over-utilization of care (which increases the number of visits needed to be treated, requiring multiple visits to different doctors and physical therapists for the same diagnosis), and getting billed for unnecessary and unproven treatments that you don’t even need. All of these factors increase cost and this is why healthcare is so expensive. We strive to end that unnecessary, expensive cycle. In fact, we are currently publishing our first-year data with the University of Central Florida that shows the cost-effectiveness of our treatment approach.
This year, the average cost of our care was shown to be $814-$1141. Some of our patients get even as low as $315 for the full treatment! So if you have a deductible of $3,000-$10,000 and you have to pay out of pocket for your treatment, we can save you lots of money.
Remember, every case of pain is different and not all heel pain is the same. It is hard to predict exactly how much your treatment is going to cost you. But after a thorough evaluation, we can tell you exactly what is causing your pain, how long it is going to take, what the best way to treat it will be, and exactly how much it is going to cost. We have no hidden fees, no co-pays, and no miscellaneous bills that you will be surprised by 3 months after you receive treatment. Your pain, your diagnosis, your goals, and what is best for you dictate your treatment and how much it will cost, and while it varies for every patient, treatment at Pursuit is still much more affordable than standard healthcare.
How long are sessions?
Our evaluations are always one-on-one with one of our board-certified specialists and 60-90 minutes long. We like to perform thorough evaluations so we can solve the root cause of your pain, identify all risk factors, and make sure that we do it right. After the evaluation, you will know your diagnosis, the root cause of why you have your pain and symptoms, your prognosis, an expected timeline of when you should see results, what the best way to treat your pain is, how much it will cost, and your expected recovery outcome. We want you to fully understand everything about your pain and injury. What is best for you and will get you the best outcome is what will dictate your care and treatment. There will be plenty of time for you to ask questions so we can make sure you fully understand why you have your pain and what the best way to treat it will be. After the evaluation is completed, all treatment sessions are 60 minutes going forward and still one-on-one with your physical therapist. You and your physical therapist will design a customized treatment plan that works for you and that will achieve your goals.
How can it be prevented?
Maintaining core and lower extremity strength and flexibility and monitoring your activity best prevents ITBS. It is important to modify your activity and contact your physical therapist soon after first feeling pain. Research indicates that when soft tissues are irritated and the offending activity is continued, the body does not have time to repair the injured area. This often leads to persistent pain, and the condition becomes more difficult to resolve. Once you are involved in a rehabilitation program, your physical therapist will help you determine when you are ready to progress back to your previous activity level. He or she will make sure that your body is ready to handle the demands of your activities so that your injury does not return. You will also receive a program to perform at home that will help you maintain the improvements that you gained during rehabilitation.
What are the next steps?
Getting started is simple. The first step and the key to getting you pain-free again
Solve the root cause of your pain
How Our Treatment is Different
We believe that working with a specific specialist for your care is the best way to solve the root cause of your pain. Work one-on-one with a Doctor of Physical Therapy every time your visit our office.
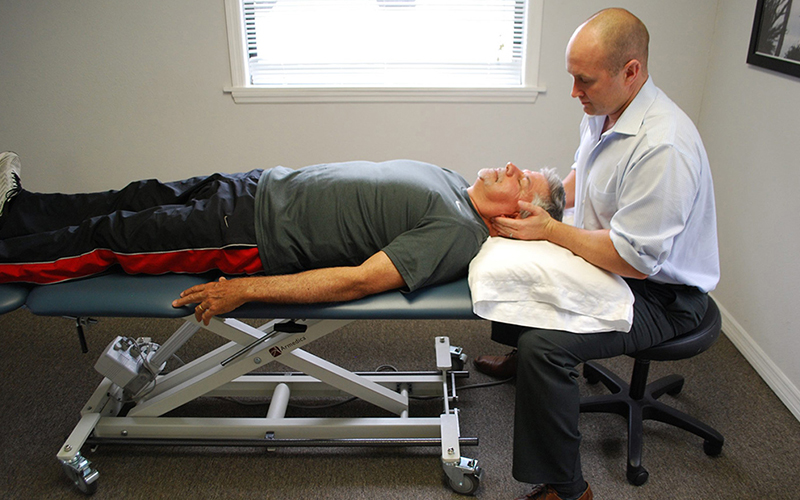
Exclusive one-on-one patient care
While most clinics will give you a limited amount of time with your Doctor, we believe that true results come from consistent one-on-one therapy.
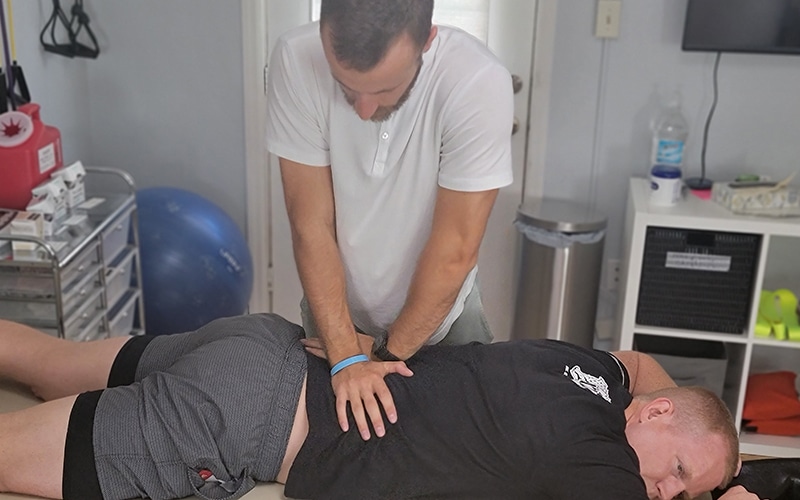
Work with your specialist every visit
Stop being handed off to trainees or non-Doctors for your Physical Therapy. At Pursuit, you'll work exclusively with your Doctor of Physical Therapy that specializes in your specific needs.
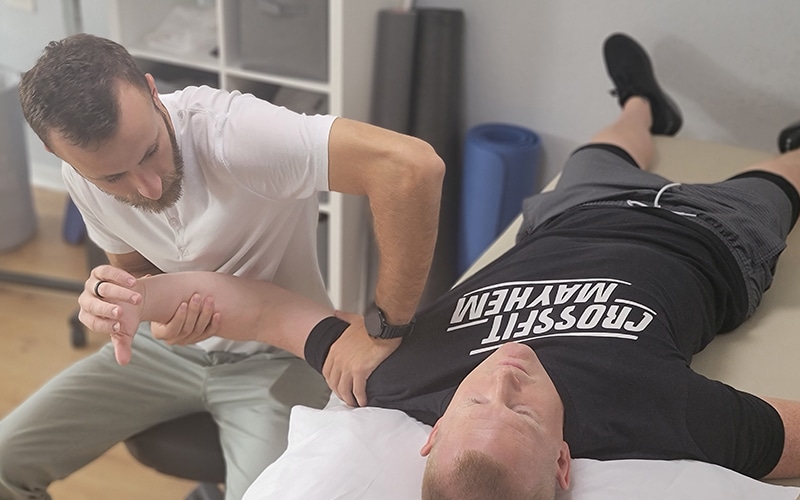
24/7 messaging access to your specialist
Ever have an issue or questions? We're here to help. Get 24/7 access to your specialist while you're under our care. Physical Therapy doesn't just happen when you're in our clinic, so we're here for you when you need us.
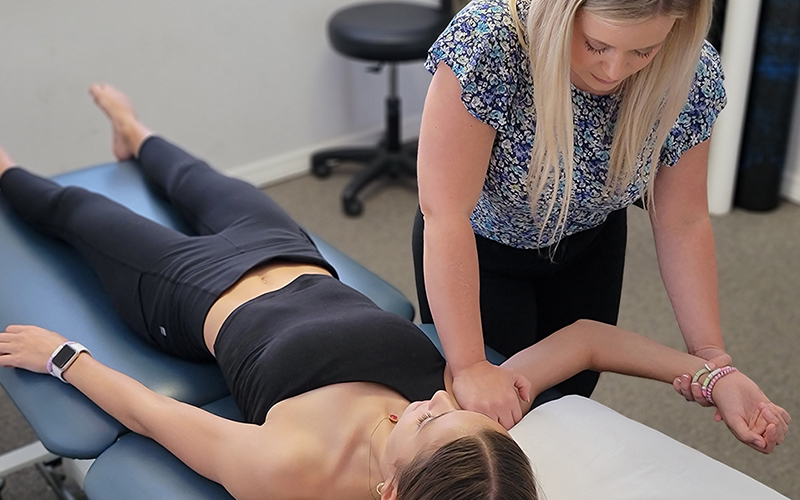
No waiting periods
Get off that waiting list and get the treatment you need. We're always ready to accept new patients, so you can get better faster and get back to a pain-free life that you deserve.
Not limited by insurance
Don't let the insurance companies tell you how much treatment you need. Avoid the limitations of short sessions that insurance provides and work with our Doctors when you need it and for as long as you need it.
No painful injections, no expensive medications, no surgery
In order to truly solve your pain, we use a holistic approach to Physical Therapy, not relying on injections, medications, or surgery. Instead, we'll strengthen your body's weak points that are causing your pain.
MEET THE TEAM

RON MILLER, DPT, OCS, Cert DN
Doctor of Physical Therapy | Board Certified Orthopaedic Physical Therapy Clinical Specialist | Post-Doctoral Orthopaedic Residency Trained | Certified in Dry Needling | Titleist Performance Institute Certified
Dr. Ron Miller is the owner and founder of Pursuit Physical Therapy. His core belief is that it is not about the physician, the physical therapist, or the insurance company: it is about what is truly best for the patient. Dr. Miller started...

MARYANN DANIELS, PT, MCMT, IDN
Physical Therapist | Dry Needling Certified | Mastery Certified In Manual Therapy | Pelvic Floor And Post Partum Specialist
Maryann was originally born in Connecticut but moved to Florida with her family at the age of 9 and she grew up in Jupiter, Florida. She then went to college at the University of Central Florida...


MICHAEL FABRICK, DPT, Cert. DN
Doctor of Physical Therapy | Certified in Dry Needling | Pursuit Sports Performance Specialist | Professional Tennis Tour Physical Therapist
Dr. Michael Fabrick was born and raised in Hanover, Pennsylvania and attended Slippery Rock University where he received his Bachelor’s degree in Exercise Science. He then went on to receive his Doctorate Degree in Physical Therapy in May of 2020. During his final tenure as a Doctoral intern, he trained underneath Todd Ellenbecker, who is one of the world’s leading experts on shoulder rehabilitation and is the Vice President of Medical Services for the ATP World Tour...

THOMAS EBERLE, DPT, FAAOMPT
Doctor Of Physical Therapy | Fellow, American Academy Of Orthopedic Manual Physical Therapist | Dry Needling Certified |
Dr. Thomas Eberle is a native of Buffalo, New York where he completed his Master of Science, Physical Therapy from D’Youville College. Dr. Eberle went on and further completed his Doctor of Physical Therapy, an Orthopedic Residency, and a Fellowship program...

BECOMING PAINFREE IS EASIER THAN YOU THINK

Step 1:
Call our expert team.
Step 2:
We’ll work with you to find and treat the root of your pain.

Step 3:
Get back to doing what you love.

 Megan
Megan Lisa B.
Lisa B.